mrpein
Bronze
- Joined
- Jan 22, 2026
- Posts
- 362
- Reputation
- 205
Peptides That Regulate Intestinal Growth
One of the key signals for intestinal growth is GLP-2. This peptide is made in the intestine when we eat and encourages growth and repair in the intestinal lining.
GLP-2 attaches to specific receptors on the surface of intestinal cells. When this happens, signaling pathways inside the cell are activated. This increases cell division, strengthens the intestinal barrier, and promotes growth of the intestinal lining.
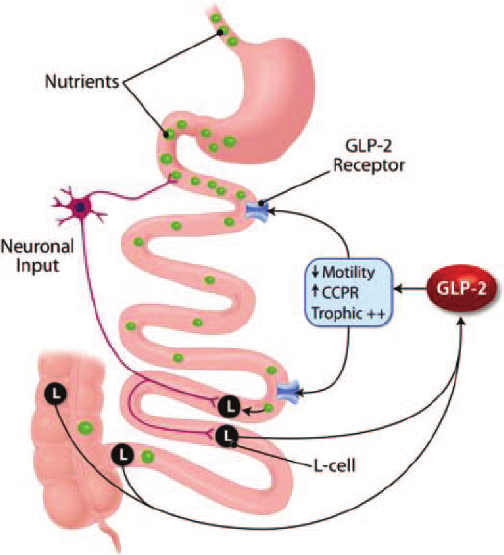
Research indicates that GLP-2 can lengthen the villi and increase the intestine's absorptive surface. Clinical studies in patients with impaired intestinal function show that treatments mimicking GLP-2 can improve nutrient absorption by 10 to 12%, along with thicker intestinal lining. In some experimental models, the total absorptive surface area of the small intestine has increased by 25 to 30% as both villi and intestinal tissue develop more.
When this signaling pathway works well, the intestine can repair itself more quickly and maintain a structure that supports efficient nutrient absorption. Studies also show that GLP-2 can boost intestinal blood flow by about 20%, which may improve the transport of absorbed nutrients to the rest of the body.
Peptides and Intestinal Healing
Another peptide often mentioned in research is BPC-157. It has been studied in animal experiments and seems to help repair injuries in the stomach and intestines.
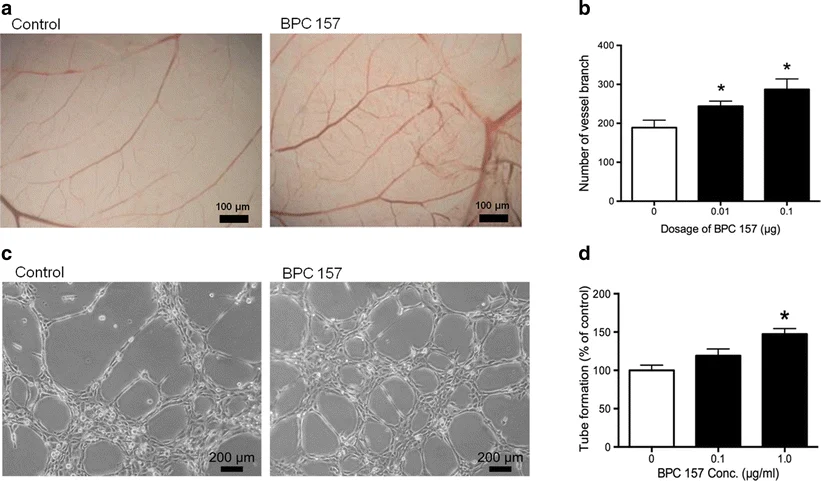
Research suggests that this peptide affects signaling pathways linked to blood vessel growth, cell movement, and tissue repair. When BPC-157 interacts with these biological systems, it can activate processes involved in healing and tissue regeneration.
Experimental studies indicate that injuries in gastrointestinal tissue may heal 30 to 40% faster when these repair mechanisms are activated. This does not necessarily mean that new villi are formed in healthy individuals, but it may aid recovery when intestinal tissue is damaged.
It is important to understand that this area of research is still evolving, and much of the current knowledge is based on experimental studies.
How This May Affect Metabolism
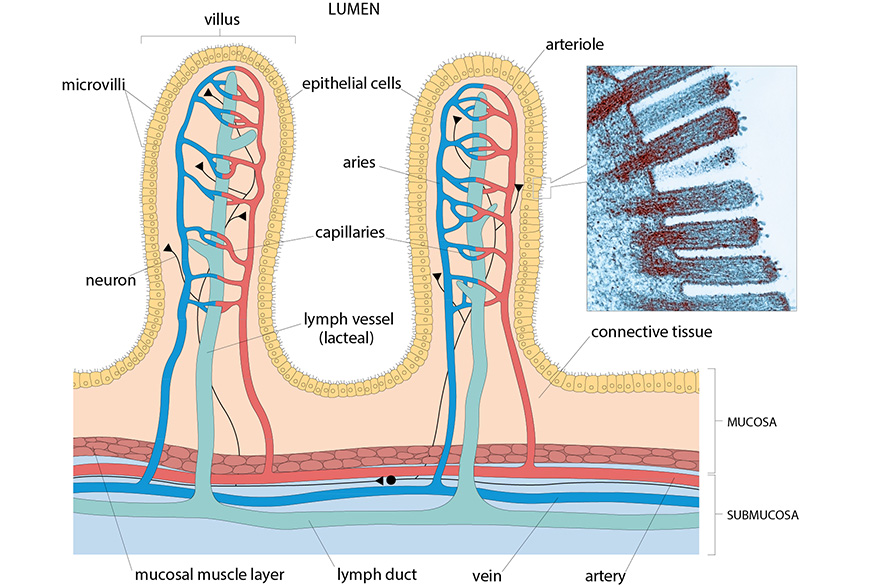
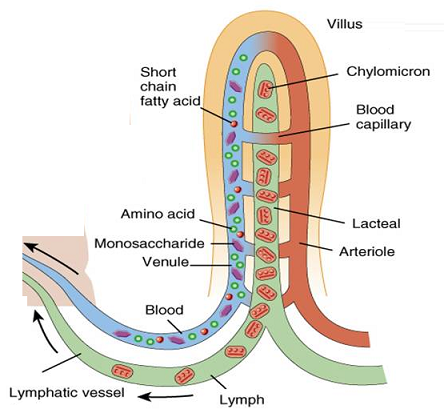
When the intestine works optimally and the villi are healthy, the body can absorb nutrients efficiently. This can impact metabolism because cells gain better access to energy and essential building blocks.
Nutrients absorbed in the intestine are used to:
- produce energy in cells
- build hormones
- repair tissues
- regulate the immune system
When nutrient absorption is effective, metabolism can stay stable because the body continuously gets the fuel it needs. Studies suggest that even small improvements in absorptive capacity can boost the body’s availability of certain nutrients by 5 to 15%. This may impact energy production and hormonal balance.
At the same time, a larger absorptive surface means the body might absorb more energy from food. In some cases, this can influence overall energy balance and how energy is stored in the body.
Chatpgt was only used as the translater as the original was typed in Swedish.
One of the key signals for intestinal growth is GLP-2. This peptide is made in the intestine when we eat and encourages growth and repair in the intestinal lining.
GLP-2 attaches to specific receptors on the surface of intestinal cells. When this happens, signaling pathways inside the cell are activated. This increases cell division, strengthens the intestinal barrier, and promotes growth of the intestinal lining.

Research indicates that GLP-2 can lengthen the villi and increase the intestine's absorptive surface. Clinical studies in patients with impaired intestinal function show that treatments mimicking GLP-2 can improve nutrient absorption by 10 to 12%, along with thicker intestinal lining. In some experimental models, the total absorptive surface area of the small intestine has increased by 25 to 30% as both villi and intestinal tissue develop more.
When this signaling pathway works well, the intestine can repair itself more quickly and maintain a structure that supports efficient nutrient absorption. Studies also show that GLP-2 can boost intestinal blood flow by about 20%, which may improve the transport of absorbed nutrients to the rest of the body.


Peptides and Intestinal Healing
Another peptide often mentioned in research is BPC-157. It has been studied in animal experiments and seems to help repair injuries in the stomach and intestines.
Research suggests that this peptide affects signaling pathways linked to blood vessel growth, cell movement, and tissue repair. When BPC-157 interacts with these biological systems, it can activate processes involved in healing and tissue regeneration.
Experimental studies indicate that injuries in gastrointestinal tissue may heal 30 to 40% faster when these repair mechanisms are activated. This does not necessarily mean that new villi are formed in healthy individuals, but it may aid recovery when intestinal tissue is damaged.
It is important to understand that this area of research is still evolving, and much of the current knowledge is based on experimental studies.

How This May Affect Metabolism
When the intestine works optimally and the villi are healthy, the body can absorb nutrients efficiently. This can impact metabolism because cells gain better access to energy and essential building blocks.
Nutrients absorbed in the intestine are used to:
- produce energy in cells
- build hormones
- repair tissues
- regulate the immune system
When nutrient absorption is effective, metabolism can stay stable because the body continuously gets the fuel it needs. Studies suggest that even small improvements in absorptive capacity can boost the body’s availability of certain nutrients by 5 to 15%. This may impact energy production and hormonal balance.
At the same time, a larger absorptive surface means the body might absorb more energy from food. In some cases, this can influence overall energy balance and how energy is stored in the body.
Chatpgt was only used as the translater as the original was typed in Swedish.