zeke.htn
Iron
- Joined
- Dec 10, 2025
- Posts
- 131
- Reputation
- 170
Table of Contents
I. Introduction
II. The maxilla as the control node of the circummaxillary complex
III. Orthodontics relative to other determinants of facial form
IV. Expansion modalities and force resolution
V. Skeletal expansion vs dentoalveolar camouflage
VI. Sutural mechanics and downstream facial effects
VII. Individual requirements, constraints, and indications
VIII. Functional environment and stabilization
IX. Observed patterns
X. Conclusion
XI. Sources
I. Guide
I. Introduction
II. The maxilla as the control node of the circummaxillary complex
III. Orthodontics relative to other determinants of facial form
IV. Expansion modalities and force resolution
V. Skeletal expansion vs dentoalveolar camouflage
VI. Sutural mechanics and downstream facial effects
VII. Individual requirements, constraints, and indications
VIII. Functional environment and stabilization
IX. Observed patterns
X. Conclusion
XI. Sources
I. Guide
Introduction
This is a full guide to ascend with orthodontics. Most conversations about orthodontics never move past teeth, and even most expansion discussions stop at palatal width. That framing is incomplete. The maxilla is not important because it widens an arch. It’s important because it sits at the center of the circummaxillary sutural system and distributes orthopedic force through the midface.
When expansion produces facial change, it isn’t incidental or cosmetic. It’s the predictable result of loading sutures that define midface width, orientation, and support. When it doesn’t, it’s usually because force never left the dentoalveolar system.
This is not a post about whether orthodontics can change the face. That question is already settled. This is about when it does, why it does, and who it actually applies to.
All claims here are grounded in CBCT evidence, sutural biology, and repeatable biomechanical patterns, not surface-level before-and-after photos.[/ISPOILER]
---
II. The maxilla as the control node of the circummaxillary complex
---
III. Orthodontics relative to other determinants of facial form
---
IV. Expansion modalities and force resolution
---
V. Skeletal expansion vs dentoalveolar camouflage
---
VI. Sutural mechanics and downstream facial effects
---
VII. Individual requirements, constraints, and indications
---
VIII. Functional environment and stabilization
---
IX. Observed patterns
---
X. Conclusion
---
XI. Sources
This is a full guide to ascend with orthodontics. Most conversations about orthodontics never move past teeth, and even most expansion discussions stop at palatal width. That framing is incomplete. The maxilla is not important because it widens an arch. It’s important because it sits at the center of the circummaxillary sutural system and distributes orthopedic force through the midface.
When expansion produces facial change, it isn’t incidental or cosmetic. It’s the predictable result of loading sutures that define midface width, orientation, and support. When it doesn’t, it’s usually because force never left the dentoalveolar system.
This is not a post about whether orthodontics can change the face. That question is already settled. This is about when it does, why it does, and who it actually applies to.
All claims here are grounded in CBCT evidence, sutural biology, and repeatable biomechanical patterns, not surface-level before-and-after photos.[/ISPOILER]
---
II. The maxilla as the control node of the circummaxillary complex
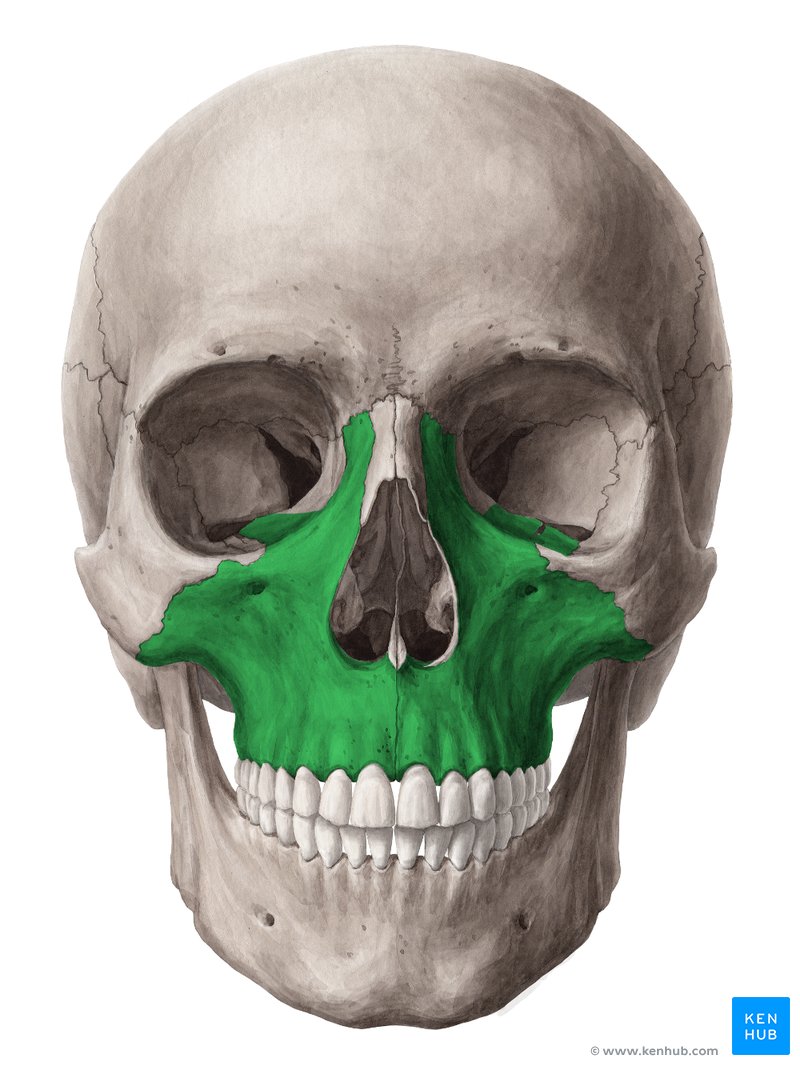
The maxilla articulates with nearly every structurally relevant facial bone. Beyond the midpalatal suture, it interfaces with the zygomatic bones, nasal bones, frontal bone, palatine bones, vomer, and indirectly the sphenoid through the pterygopalatine region.
Because of this, the maxilla functions as a load distributor. Once sufficient force overcomes dentoalveolar resistance and initiates sutural displacement, that force propagates through the circummaxillary system, especially the zygomaticomaxillary, frontomaxillary, nasomaxillary, and pterygopalatine sutures.
This is why true skeletal expansion is never purely transverse. It is a three-dimensional displacement constrained by cranial base anchorage and sutural interdigitation. Faces change not because bone “grows,” but because spatial relationships within the craniofacial complex are altered.

Because of this, the maxilla functions as a load distributor. Once sufficient force overcomes dentoalveolar resistance and initiates sutural displacement, that force propagates through the circummaxillary system, especially the zygomaticomaxillary, frontomaxillary, nasomaxillary, and pterygopalatine sutures.
This is why true skeletal expansion is never purely transverse. It is a three-dimensional displacement constrained by cranial base anchorage and sutural interdigitation. Faces change not because bone “grows,” but because spatial relationships within the craniofacial complex are altered.
---
III. Orthodontics relative to other determinants of facial form
From a structural hierarchy standpoint:
Cranial base orientation → maxillary position and width → mandibular posture → dental expression
Orthodontics only becomes facially relevant when it interacts upstream of the dentition. Dentoalveolar changes occur downstream and do not reorganize facial constraints.
This explains why identical occlusal outcomes can coexist with radically different facial outcomes. One case altered skeletal boundaries. The other optimized within them.
Cranial base orientation → maxillary position and width → mandibular posture → dental expression
Orthodontics only becomes facially relevant when it interacts upstream of the dentition. Dentoalveolar changes occur downstream and do not reorganize facial constraints.
This explains why identical occlusal outcomes can coexist with radically different facial outcomes. One case altered skeletal boundaries. The other optimized within them.
---
IV. Expansion modalities and force resolution
The meaningful distinction between expansion systems is not speed or branding, but where force resolves.
Removable and tooth-borne expanders dissipate force into alveolar bone and the periodontal ligament. Outside early childhood, skeletal engagement is minimal.
Facemask therapy loads the circummaxillary sutures anteriorly, targeting forward displacement of the maxilla. Its effectiveness is dictated by sutural patency and timing, not compliance alone.
MARPE introduces skeletal anchorage but still loses a significant portion of force dentally. In mature patients, sutural opening is often incomplete or non-parallel.
MSE is engineered to bypass alveolar dissipation and engage both maxillary cortices. When successful, force transmits laterally into the zygomatic buttresses and posteriorly toward the pterygopalatine region, producing effects beyond the dental arch.
MASPE attempts to further refine vector control, but the underlying principle remains identical: maximize sutural loading and minimize dentoalveolar loss.
The appliance is not the treatment. The force distribution is.
Removable and tooth-borne expanders dissipate force into alveolar bone and the periodontal ligament. Outside early childhood, skeletal engagement is minimal.
Facemask therapy loads the circummaxillary sutures anteriorly, targeting forward displacement of the maxilla. Its effectiveness is dictated by sutural patency and timing, not compliance alone.
MARPE introduces skeletal anchorage but still loses a significant portion of force dentally. In mature patients, sutural opening is often incomplete or non-parallel.
MSE is engineered to bypass alveolar dissipation and engage both maxillary cortices. When successful, force transmits laterally into the zygomatic buttresses and posteriorly toward the pterygopalatine region, producing effects beyond the dental arch.
MASPE attempts to further refine vector control, but the underlying principle remains identical: maximize sutural loading and minimize dentoalveolar loss.
The appliance is not the treatment. The force distribution is.
---
V. Skeletal expansion vs dentoalveolar camouflage
Dentoalveolar expansion increases arch perimeter while preserving facial constraints. Skeletal expansion alters the constraints themselves.
Camouflage presents as:
* Buccal tipping
* Cortical thinning
* Minimal nasal or midface response
* High relapse risk
Skeletal response presents as:
* Midpalatal separation
* Lateral displacement of the zygomatic buttresses
* Increased nasal volume
* Secondary mandibular repositioning
This distinction is obvious on CBCT and ambiguous in photographs, which is why confusion persists.
Camouflage presents as:
* Buccal tipping
* Cortical thinning
* Minimal nasal or midface response
* High relapse risk
Skeletal response presents as:
* Midpalatal separation
* Lateral displacement of the zygomatic buttresses
* Increased nasal volume
* Secondary mandibular repositioning
This distinction is obvious on CBCT and ambiguous in photographs, which is why confusion persists.
---
VI. Sutural mechanics and downstream facial effects
Zygomatic complex: Force transmitted through the zygomaticomaxillary sutures alters the spatial relationship between the midface and cranial base. This expresses as increased midface width and lateral support, not literal cheekbone growth.
CCW mandibular rotation: Expansion does not rotate the mandible directly. Improved airway volume and tongue posture shift the functional equilibrium, allowing counterclockwise adaptation in susceptible cases.
Orbital support: The maxilla contributes to the inferior orbital rim and floor. Sutural displacement can improve under-eye support subtly. Claims beyond this require imaging, not anecdote.
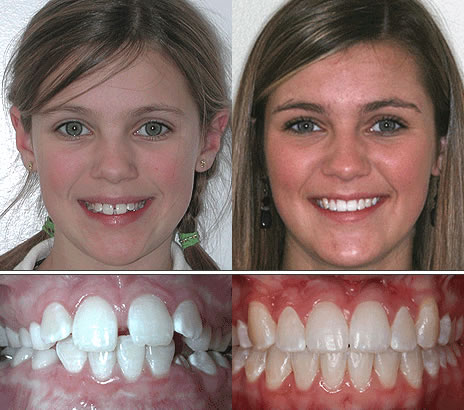
Smile expression: A widened skeletal base allows teeth to upright into a broader arc without compensatory flaring, improving smile fullness and lip support.

CCW mandibular rotation: Expansion does not rotate the mandible directly. Improved airway volume and tongue posture shift the functional equilibrium, allowing counterclockwise adaptation in susceptible cases.
Orbital support: The maxilla contributes to the inferior orbital rim and floor. Sutural displacement can improve under-eye support subtly. Claims beyond this require imaging, not anecdote.
Smile expression: A widened skeletal base allows teeth to upright into a broader arc without compensatory flaring, improving smile fullness and lip support.
---
VII. Individual requirements, constraints, and indications
Expansion is not universal. Outcomes depend on starting constraints.
Key variables:
* Age and sutural maturation
* Maxillary width versus AP position
* Vertical growth pattern
* Mandibular posture
* Airway status and breathing mode
* Degree of existing dentoalveolar compensation
Narrow maxilla, adequate AP position
Best indication for skeletal expansion. Typically responds with improved interzygomatic width, better nasal airflow, and subtle CCW mandibular adaptation. Expansion alone is often sufficient.
Narrow and retrusive maxilla
Expansion alone addresses width but not projection. Without AP correction, transverse gain may exaggerate midface flatness. These cases require controlled vector planning and often protraction earlier in life.
Vertically excessive patterns
High-angle cases are sensitive to force direction. Poorly controlled expansion can worsen facial length. When airway and function improve, CCW adaptation is possible, but this is conditional, not guaranteed.
Adolescents versus adults
In adolescents, circummaxillary sutures retain plasticity and respond more globally. In adults, midpalatal separation may occur, but circummaxillary resistance limits facial change. Expectations should be structural, not transformational.
Dentoalveolar compensation-dominant cases
Flared teeth and thin cortical plates often indicate compensation rather than true skeletal deficiency. Expansion here is frequently unnecessary or harmful. Decompensation may be the correct move.
Perfect example of someone who needs expansion:

Key variables:
* Age and sutural maturation
* Maxillary width versus AP position
* Vertical growth pattern
* Mandibular posture
* Airway status and breathing mode
* Degree of existing dentoalveolar compensation
Narrow maxilla, adequate AP position
Best indication for skeletal expansion. Typically responds with improved interzygomatic width, better nasal airflow, and subtle CCW mandibular adaptation. Expansion alone is often sufficient.
Narrow and retrusive maxilla
Expansion alone addresses width but not projection. Without AP correction, transverse gain may exaggerate midface flatness. These cases require controlled vector planning and often protraction earlier in life.
Vertically excessive patterns
High-angle cases are sensitive to force direction. Poorly controlled expansion can worsen facial length. When airway and function improve, CCW adaptation is possible, but this is conditional, not guaranteed.
Adolescents versus adults
In adolescents, circummaxillary sutures retain plasticity and respond more globally. In adults, midpalatal separation may occur, but circummaxillary resistance limits facial change. Expectations should be structural, not transformational.
Dentoalveolar compensation-dominant cases
Flared teeth and thin cortical plates often indicate compensation rather than true skeletal deficiency. Expansion here is frequently unnecessary or harmful. Decompensation may be the correct move.
Perfect example of someone who needs expansion:
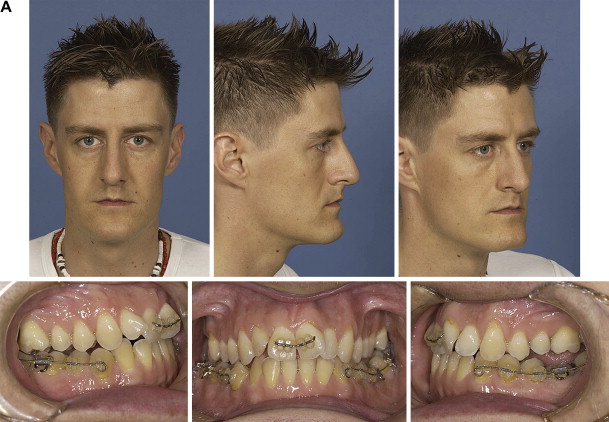
---
VIII. Functional environment and stabilization
Sutures adapt under load but stabilize under function.
Without nasal breathing, palatal tongue posture, and closed-mouth rest position, relapse pressure remains constant. Expansion fails not because sutures close, but because functional forces never realign to support the new configuration.
Orthodontics sets boundary conditions. Function determines equilibrium.
Without nasal breathing, palatal tongue posture, and closed-mouth rest position, relapse pressure remains constant. Expansion fails not because sutures close, but because functional forces never realign to support the new configuration.
Orthodontics sets boundary conditions. Function determines equilibrium.
---
IX. Observed patterns
Meaningful facial change correlates with:
* Multisutural engagement rather than isolated midpalatal opening
* Force magnitude sufficient to overcome circummaxillary resistance
* Residual sutural plasticity
* A post-treatment functional environment that reinforces expansion
Cases that disappoint aesthetically almost always succeed dentally.
* Multisutural engagement rather than isolated midpalatal opening
* Force magnitude sufficient to overcome circummaxillary resistance
* Residual sutural plasticity
* A post-treatment functional environment that reinforces expansion
Cases that disappoint aesthetically almost always succeed dentally.
---
X. Conclusion
Orthodontics alters faces only when it alters constraints. The maxilla matters not because it holds teeth, but because it distributes force through a sutural system that defines midface structure.
If sutures are not meaningfully engaged, facial change is incidental.
If they are, it is structural.
If sutures are not meaningfully engaged, facial change is incidental.
If they are, it is structural.
---
XI. Sources
Angelieri F, Cevidanes LHS, Franchi L, Gonçalves JR, Benavides E, McNamara JA. Midpalatal suture maturation: classification method for individual assessment before rapid maxillary expansion. American Journal of Orthodontics and Dentofacial Orthopedics. 2013;144(5):759–769.
Cantarella D, Dominguez-Mompell R, Moschik C, et al. Changes in the midfacial complex following maxillary skeletal expander (MSE) therapy: a CBCT study. Progress in Orthodontics. 2017;18(1):1–11.
Enlow DH, Hans MG. Essentials of Facial Growth. Philadelphia: W.B. Saunders; 1996.
Proffit WR, Fields HW, Larson BE, Sarver DM. Contemporary Orthodontics. 6th ed. St. Louis: Elsevier; 2019.
Carlson DS. Sutural growth of the craniofacial skeleton. In: McNamara JA, ed. Determinants of Mandibular Form and Growth. Ann Arbor: University of Michigan; 1984.
Cantarella D, Dominguez-Mompell R, Moschik C, et al. Changes in the midfacial complex following maxillary skeletal expander (MSE) therapy: a CBCT study. Progress in Orthodontics. 2017;18(1):1–11.
Enlow DH, Hans MG. Essentials of Facial Growth. Philadelphia: W.B. Saunders; 1996.
Proffit WR, Fields HW, Larson BE, Sarver DM. Contemporary Orthodontics. 6th ed. St. Louis: Elsevier; 2019.
Carlson DS. Sutural growth of the craniofacial skeleton. In: McNamara JA, ed. Determinants of Mandibular Form and Growth. Ann Arbor: University of Michigan; 1984.
Last edited: