Finntrado
retard
- Joined
- Feb 8, 2026
- Posts
- 68
- Reputation
- 36
SO before I begin this post, i know a lot of information contained in this has already been published on the forum but i just wanted to gather all the data together and present it in a neat manner for those who are interested in eyelightening methods that MIGHT actually work.
Topical beta blockers like levobunolol and systemic fluoroquinolones such as moxifloxacin have been linked to iris depigmentation across multiple case reports. This can lighten eye color by reducing stromal melanin. This means there's a chance create that normies with dark irises can enhance their eye area, and gain a massive halo. This theory suggests that these drugs interfere with melanin pathways, causing aesthetic changes from T50+ tiers to lighter shades (from slight to straight up blue eyes).
Practical Implications
So basically long term use of topical beta blockers and moxifloxacin might help gradually lighten the color of brown eyes to THEORETICALLY achieve an A10-A20 halo effect, though results may vary however I'd assume no matter what you should be able to lighten your eyes to some degree on this stack. Combining these drugs with prostaglandin analogs may prevent rebound effects, or melanin inhibitors could enhance results. However, it is best to start with a low dose and monitor IOP and vision. These methods may work well for long-term protocols in T50+ betas aiming for effects similar to heterochromia or just eye lightening in general.
Limitations/Risks
Depigmentation is rare and has often appeared only in isolated cases. It might be coincidental with age aswell or infection rather than a direct result of the medications. For example, moxifloxacin may be the consequence of post-respiratory injury/disease. Changes can persist after stopping the medication, leading to potential glare or light sensitivity without reversal. Differences between topical and systemic applications also limit their generalizability, and there are no controlled studies on this topic. And obviously putting shit in your eyes generally can't go well, same goes for taking medicine without being sick, but it's not like there's a major downside so atp just fuck it and go for it ngl.
Topical beta blockers like levobunolol and systemic fluoroquinolones such as moxifloxacin have been linked to iris depigmentation across multiple case reports. This can lighten eye color by reducing stromal melanin. This means there's a chance create that normies with dark irises can enhance their eye area, and gain a massive halo. This theory suggests that these drugs interfere with melanin pathways, causing aesthetic changes from T50+ tiers to lighter shades (from slight to straight up blue eyes).
Iris pigmentation depends on melanin found in stromal melanocytes. Depigmentation lowers stromal density, revealing underlying structures and resulting in a lighter appearance. For levobunolol, which is a non-selective beta blocker, long-term use mimics Horner's syndrome by blocking sympathetic tone. This lowers catecholamine levels, which may reduce prostaglandin production and disrupt melanin maintenance. Basically taking levobunolol causes a chronic low-sympathetic state in the iris → gradual stromal melanin loss → lighter eye color over years. This theory suggests this aligns with prostaglandin analogs like latanoprost, which prevent hypopigmentation in animal models and indicate that prostaglandins help maintain baseline melanin.
In contrast, moxifloxacin, when used shortly after an infection, causes pigment dispersion, possibly through tyrosinase inhibition or inflammatory damage to melanocytes. This leads to transillumination and abnormal eye color. Both drugs affect TYR-mediated melanin production, but beta blockers have a long-term effect via neural pathways, while quinolones provoke quick, but still lasting and possibly immune-related changes.
In contrast, moxifloxacin, when used shortly after an infection, causes pigment dispersion, possibly through tyrosinase inhibition or inflammatory damage to melanocytes. This leads to transillumination and abnormal eye color. Both drugs affect TYR-mediated melanin production, but beta blockers have a long-term effect via neural pathways, while quinolones provoke quick, but still lasting and possibly immune-related changes.

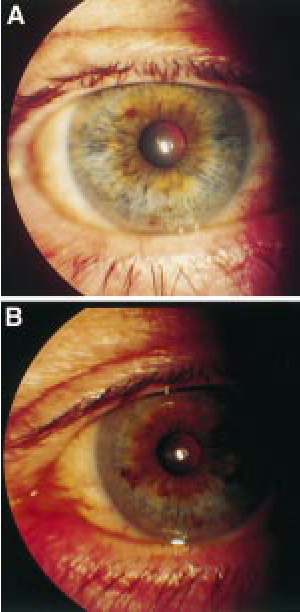
In a case involving a 68-year-old man, after five years of using twice-daily drops for ocular hypertension (IOP 32 mm Hg OU), his irises changed from brown to blue. His central brown stroma and naevi remained intact. There was no atrophy, transillumination, pigment dispersion, or inflammation, and his vision was preserved (6/5 OD, 6/6 OS). The authors speculated about a pharmacological Horner's effect, referring to rabbit studies where prostaglandins influence pigmentation and changes in IOP.
https://www.researchgate.net/publication/12655182_A_case_of_acquired_iris_depigmentation_as_a_possible_complication_of_levobunolol_eye_drops
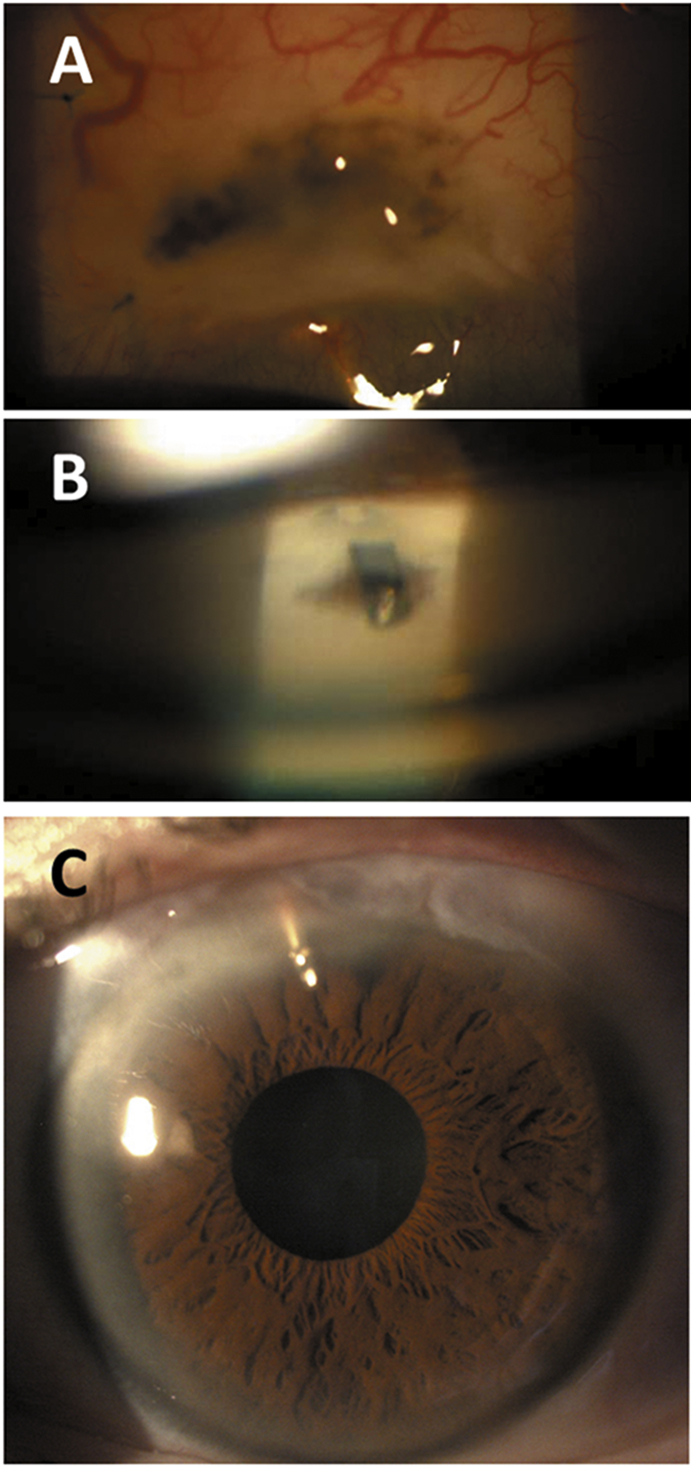
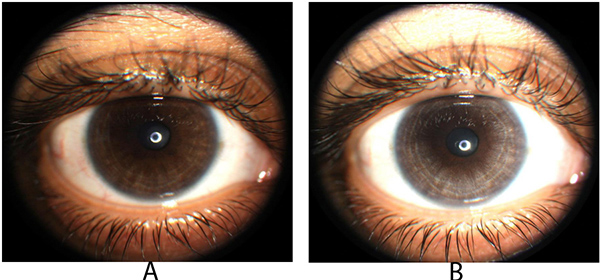
In several moxifloxacin cases involving a 70-year-old woman, a 32-year-old woman, and a 26-year-old man, systemic use for pneumonia or respiratory infections caused depigmentation within 2-3 months. Symptoms included bilateral asymmetrical transillumination, abnormal eye color, and light sensitivity; one patient had a mild anterior chamber reaction that resolved with steroids. Vision and IOP were normal, with no keratic precipitates or synechiae. Their conditions were distinguishable from Fuchs' syndrome (which shows diffuse atrophy) or herpetic iridocyclitis (characterized by sectoral atrophy and increased IOP). The patients’ eye status was relevant because oral medication tends to accumulate in the aqueous humor. A case of parvovirus uveitis in a 6-year-old girl illustrates infection-related autoimmunity mimicking depigmentation but resolving without changing eye color, indicating other non-drug factors at play.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7057145/
https://openophthalmologyjournal.com/VOLUME/11/PAGE/107/FULLTEXT/


1. Levobunolol (Topical Beta Blocker - e.g., Betagan 0.5% solution)
- Standard therapeutic dosage (for glaucoma/ocular hypertension):
- 0.5% solution: 1–2 drops in affected eye(s) once daily (starting dose).
- Can increase to twice daily if IOP not controlled (more severe cases).
- 0.25% solution alternative: 1–2 drops twice daily.
- Doses >1 drop twice daily usually not more effective (therapeutically speaking).
- In depigmentation case report:
- Bilateral use: Twice daily (BID) for 5 years exclusively (no other drops).
- Patient (68M) self-reported gradual brown-to-blue shift after long-term exposure.
- No concentration specified in the 1999 BJO letter, but standard 0.5% assumed based on era/common formulations.
- Standard therapeutic dosage (for pneumonia/respiratory infections):
- 400 mg orally once daily.
- Duration: 7–14 days for community-acquired pneumonia; 5–10 days for acute bacterial sinusitis or exacerbations of chronic bronchitis.
- In depigmentation case reports(from 2013 Clinics letter and related):
- Case 1 (70F): 15-day course for pneumonia → symptoms 3 months post-treatment.
- Case 2 (32F): Course for pneumonia (duration not specified) → symptoms 2 months post.
- Case 3 (26M): Course for upper respiratory infection (duration not specified) → symptoms 3 months post.
Practical Implications
So basically long term use of topical beta blockers and moxifloxacin might help gradually lighten the color of brown eyes to THEORETICALLY achieve an A10-A20 halo effect, though results may vary however I'd assume no matter what you should be able to lighten your eyes to some degree on this stack. Combining these drugs with prostaglandin analogs may prevent rebound effects, or melanin inhibitors could enhance results. However, it is best to start with a low dose and monitor IOP and vision. These methods may work well for long-term protocols in T50+ betas aiming for effects similar to heterochromia or just eye lightening in general.
Limitations/Risks
Depigmentation is rare and has often appeared only in isolated cases. It might be coincidental with age aswell or infection rather than a direct result of the medications. For example, moxifloxacin may be the consequence of post-respiratory injury/disease. Changes can persist after stopping the medication, leading to potential glare or light sensitivity without reversal. Differences between topical and systemic applications also limit their generalizability, and there are no controlled studies on this topic. And obviously putting shit in your eyes generally can't go well, same goes for taking medicine without being sick, but it's not like there's a major downside so atp just fuck it and go for it ngl.


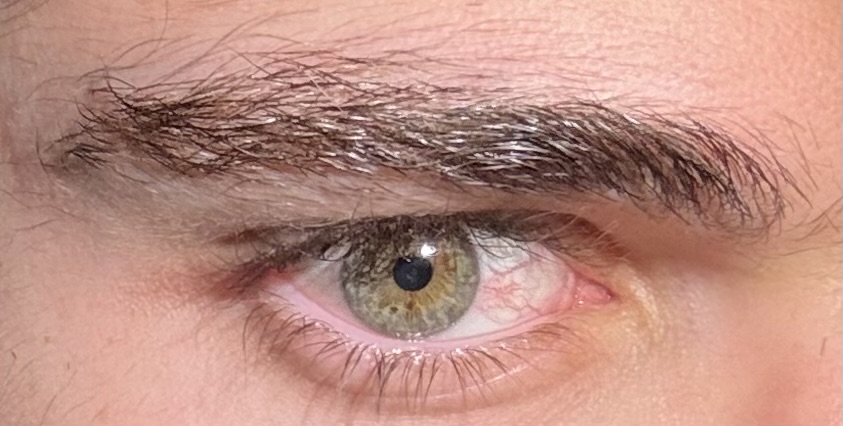

 , i'm saying that's the standard dosage for when someone has respiratory infections or pneumonia, do some research on what would be the safe amount for a healthy male or just do 400 if you really wanna deal with the sides i guess. also you might want to work on that scelera a bit it's lowk red. might be a bigger halo for you than blue eyes.
, i'm saying that's the standard dosage for when someone has respiratory infections or pneumonia, do some research on what would be the safe amount for a healthy male or just do 400 if you really wanna deal with the sides i guess. also you might want to work on that scelera a bit it's lowk red. might be a bigger halo for you than blue eyes.