Elf
Ascension
- Joined
- Sep 17, 2023
- Posts
- 1,228
- Reputation
- 1,998
DISCLAIMER
Table of Contents
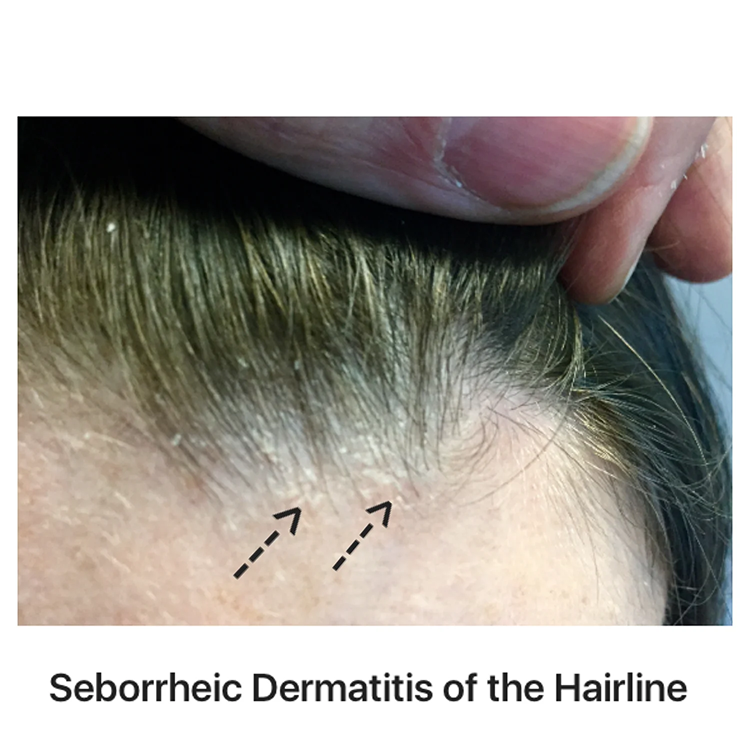
What is Seborrheic Dermatitis? We'll refer to it as "SD" in this thread
Seborrheic dermatitis is a very common chronic skin disorder causing red, greasy, and flaky patches on areas of the body (focusing on scalp here) that are richly supplied with oil producing glands. The scalp, face, and chest tend to be affected by this type of skin disease and studies currently believe it occurs due to a combination of the yeast on your skin (malassezia), excessive production of oil, as well as an inflammatory reaction, although it is not contagious and the exact mechanisms behind its development remain poorly understood. "Dandruff" can be viewed as the most mild form of the disease and it can appear at random times.
Why I am making this thread
I've had seborrheic dermatitis since the age of 13, and tried almost every treatment, product, and method for a few years in order to manage my SD. I was able to develop a reliable protocol that currently keeps my SD under control, and also helps mask many of its signs. The information I'm providing comes from extensive testing and researching many different treatments and products. To my knowledge, there are no other places online that provide all of the information I am providing here, all in one location. People that had interest in this subject may already be aware of many things here, but I haven't found a thread mentioning all of them in relation to SD.
My case
Other examples
Why does this matter?
For those affected by it, SD is one of the things that barely gets talked about in looksmaxing, even though it has a big impact on how clean, healthy, and put-together you look. Flaking, redness, and weird shines can turn anyone into a subhuman and mess with how your hair looks and even skin quality. As far as I'm aware there is no "real cure". Why? Because most of it is due to: genetics, your skin barrier & how oily your skin is naturally. (https://www.ncbi.nlm.nih.gov/books/NBK551707/)
So, with the right protocol as well as by avoiding triggers and being consistent, you can keep it under control just enough for it to stop being a noticeable looksmin and burden.
Hairloss / Balding
I started balding at 17, and one factor that may have amplified it is poorly controlled SD. If you're suffering from this condition, you need to understand that once it has been active for too long, what happens is it keeps your scalp in a state of both chronic irritation and inflammation. As many of you already know from other threads, an inflamed environment in the scalp makes it more likely to create increased oxidative stress around the follicles. This can cause hairs to shed more often or even grow less strong. This basically makes thinning look worse or progress faster, on top of pre-existing genetic hair loss. This doesn't mean "SD causes permanent baldness" by itself, but it can act like an accelerator if it's left untreated. (https://pmc.ncbi.nlm.nih.gov/articles/PMC6369642/, https://pubmed.ncbi.nlm.nih.gov/16901187/)
Note: There is no STRONG evidence that this is true, we have limited observational and correlational studies.
The Protocol Itself
Required items
Nidoflor or similar variant

I used a product called "Nidoflor", which is a combo of triamcinolone acetonide + neomycin sulfate + nystatin (per 1g: triamcinolone acetonide 1 mg = 0.1%, neomycin sulfate 3.82mg, nystatin 100,000 IU). I haven't found this exact combo being sold anywhere else, but you could find some close matches under the form of a topical cream. (SmPC of my product in Romanian)
Here's what each of these compounds are.
Nystatin: an antifungal agent
Neomycin sulfate: a topical antibiotic
Triamcinolone acetonide: a synthetic corticosteroid
Dall'Oglio et al. (2022) report that the use of topical potent corticosteroids achieves quick control of erythema, scaling, and pruritus in seborrheic dermatitis. Just note it also warns about the risks involved.
(https://pmc.ncbi.nlm.nih.gov/articles/PMC9365318/)
Itraconazole pills

I would say this was the biggest needle mover in my case. After using itraconazole pills for just about two weeks, I had already noticed a huge reduction in the intensity of my symptoms, and after 6 weeks the symptoms were almost completely gone and I had a lot less outbreaks. Both the inflammation and scaling clearly improved from baseline. My personal observation aligns with published clinical data, where "63.4% of the patients achieve clearance of the lesions, and none had severe disease", supporting the efficacy of oral itraconazole in reducing seborrheic dermatitis severity (Nguyen et al., 2019) (https://pmc.ncbi.nlm.nih.gov/articles/PMC6364731)
Ketaconazole shampoo (pref 2%+)

Barbosa V et al. (2024) reports that prescription ketoconazole shampoo (2%) is a reliable treatment for scalp SD, and is also nicely tolerated and effective at relieving symptoms. The paper actually compares ketoconazole with selenium disulphide as an alternative but we're focusing on ketoconazole. Just note that selenium disulphide was presented as a well-tolerated alternative.
(https://pubmed.ncbi.nlm.nih.gov/39659649/)
MCT Oil with C8 and C10

Papavassilis C et al. (1999) reports that medium-chain triglycerides (including C8 and C10, which my MCT oil is made of) reduced the growth of Malassezia species, suggesting potential antifungal effects relevant to conditions like SD.
From my research, this study seems to be the most recent one that directly associates MCTs with growth inhibition effects on Malassezia species. There is newer research that have explored antimicrobial and antifungal properties of medium-chain fatty acids in broader contexts, but I haven't found any that directly look into the relationship between MCTs and Malassezia growth. (https://pubmed.ncbi.nlm.nih.gov/10507598/)
Lice comb

Optional
Cleanser
 Moisturizer
Moisturizer

The Routine

We'll have an initial phase in which the goal is to quickly reduce scaling and inflammation and suppress Malassezia driven activity, then a maintenance phase to stop symptoms from returning. SD isn't always caused by simple fungal overgrowth. Malassezia is a normal part of everyone's skin's microbiome, and the condition is likely the result of a mix of: microbiome imbalance, barrier factors, and the individual's inflammatory response. The goal is symptom control and a more stable scalp environment, so don't consider it a permanent 'cure'.
Day 0
I strongly suggest getting a short haircut.
It helps the products reach the scalp much better and makes SD easier to manage.
First 14 days
Itraconazole:
200 mg/day for 14 days. Don't extend daily usage beyond this, as itraconazole can be hard on the liver.
MCT oil:
Apply to the most affected areas a few hours before showering, then wash it out so your hair doesn't stay greasy.
Daily shower routine:
Use lukewarm water and thoroughly soak the scalp.
Gently use the lice comb to lift/remove flakes so the shampoo can reach the scalp properly.
Apply the ketoconazole shampoo and let it sit for 5 minutes.
Rinse, then apply the shampoo one more time without letting it sit.
After the shower, pat your scalp with a towel (DON'T RUB, friction can worsen irritation).
While hair is still slightly damp, apply your variant of Nidoflor to the red + flaky areas and let it air-dry.
Nidoflor (your variant) duration:
Use it 7 days in a row only, since it contains a strong corticosteroid (and you don't want to become dependent on it)
Post 7 days
We stop using the Nidoflor (or the corticosteroid + antibiotic) but we keep showering everyday with the protocol above and keep using MCT Oil.
Post 14 days
Itraconazole:
200mg/week for 4 more weeks
At this point, we have reached the final stage. We have stopped using Nidoflor (your variant), and we will only use itraconazole once a week for a month. All that remains is to maintain our progress by following the protocol 3–4 times a week (MCT oil + ketoconazole 2% shampoo). It is highly recommended not to blow-dry your hair and instead to use a towel to remove as much moisture as possible.
Why do we keep using itraconazole?
Interactions with environment

Winter/Cold
SD tends to be worse/more common in winter: a study shows SD showed up more often when it was colder, and it was also more common when UV/sunlight levels were lower. A simple reason is that cold weather + dry indoor heating can weaken the scalp's protective skin barrier, making it easier for irritation and inflammation to flare. Less sunlight also matters because UV light can reduce microbes (UV is used in germicidal settings to inactivate bacteria and/or fungi). This won't matter much if you're just planning on rotting indoors for the rest of your life. Anyway, the same study notes sunlight has been shown to suppress Malassezia. Lab research also found certain near-UV wavelengths can reduce Malassezia growth in a dose-dependent way (not in this specific paper). (https://pmc.ncbi.nlm.nih.gov/articles/PMC9040311/)
Solution: Shower in lukewarm water, then a apply a gentle cleanser and a moisturizer (face + hairline/scalp edges). Check if your home has dry air with a hygrometer. If it is the case then a humidifier helps, just don't overdo it. Lastly, moderate amounts of sunlight exposure can be useful.

Air Pollution
SD can also be worse in more polluted environments: a study shows people exposed to higher levels of common air pollutants had a higher risk of developing late-onset SD. That's because pollution is basically tiny particles and irritating gases that can sit on your skin and/or scalp. While this is not a huge issue, it's part of the many things that worsen SD. If you're exposed to them for a long period of time, they just become persistent mild irritants to your scalp. That can lead to inflammation, messes up your scalp's skin barrier and also ramps up oxidative stress, so you'll be losing moisture more easily. Note that there is no direct proof that this leads to SD by itself. (https://pubmed.ncbi.nlm.nih.gov/38648509/, https://pmc.ncbi.nlm.nih.gov/articles/PMC6766865/)
Solution: Use a HEPA air purifier at home (especially in the bedroom) to reduce indoor particulate pollution, which may help lower an environmental trigger.
My personal choices for air purifiers are the Airfanta 3Pro or Levoit 300S. Keep in mind this solution is not tested in this paper specifically, it's just my reasoning, common sense and hopefully a good exposure-reduction step. Lack of evidence regarding this specific solution does not mean it won't work, especially since it carries zero risk.

Diet
Based on available studies, SD seems to have a diet connection for some people, but it's not universal. One study shows that people who ate more fruit had less SD, while a more "Western" pattern (typical processed/fast-food style) was linked to more SD (fruit pattern ~ 25% lower odds, Western pattern ~ 47% higher odds). On the other hand, a case-control study reported that almost half of SD patients (49.2%) said foods did not affected their flares. In those who noticed triggers, the most common ones were sweets, spicy and fried foods, as well as dairy. Their data also showed daily bread, rice, pasta intake was more common in the SD group. The simple explanation is that lots of refined carbs can push hormones like IGF-1, and that may increase oil production and inflammation, while fruits/vegetables patterns may help via antioxidants and overall "less inflammatory" eating. (https://pmc.ncbi.nlm.nih.gov/articles/PMC10719884/, https://pubmed.ncbi.nlm.nih.gov/30130619/)
Solution: If you want to keep it simple, you've got two choices. Either do an elimination diet, or just straight up cut refined carbs/sugar (sodas, pastry, bread). Instead, try fruits and whole foods (red meat, organs, healthy fats, vegetables). This may be personal, but pasteurized dairy specifically seemed more likely to inflame me, so I just avoid that.
Interactions with other things
Isotretinoin
Isotretinoin works by shrinking the sebaceous glands. That means they make much less sebum, and with less oil, the scalp is less of a lipid-rich environment for Malassezia (lipid-dependent), and inflammation can calm. Low-dose has been studied for moderate to severe SD.
Short term: It often causes dry skin/scalp and has been shown to weaken the protective layer of the skin, which leads to moisture evaporating from the surface and triggers an irritant retinoid rash. In our case for the scalp, this shows up as more dryness, redness, itching, and flaking, especially early on.
Long term: Over months, isotretinoin can control SD symptoms while you're still taking it, but dry skin/scalp irritation can persist. Once you stop using it, SD can relapse (one study reported ~11% recurrence within 3 months). Data suggests a dose effect: 20 mg/day may provide better control and less relapses than 10 mg/day over a longer period.
https://pubmed.ncbi.nlm.nih.gov/27778328/
https://www.jaad.org/article/S0190-9622(25)02114-0/
https://www.jaad.org/article/S0190-9622(23)01351-8/
Note: I can access the JAAD papers using my student credentials, not sure if they are accessible for free.

Finasteride/Dutasteride:
Why it might help SD: My theory was that lowering DHT could reduce androgen-driven oiliness, but in practice, a human endocrine study found finasteride "did not decrease the sebum score from baseline values". That means it may not meaningfully reduce scalp oil.
Explaining type 1 and type 2
Our bodies have two main versions of 5-alpha reductase. That's the enzyme that converts testosterone to DHT, but there are better threads explaining this in detail. Simply put, type 1 is found a lot in skin/oil glands (sebaceous) and type 2 is found in tissues like hair follicles, prostate, etc. For our topic, the difference does matter, because blocking the version that's more active in oil glands is in theory more likely to affect skin/scalp oiliness.
Finasteride: mainly blocks type 2, that means, it lowers DHT in type 2 dominant tissues, but it's less likely to significantly reduce scalp sebum (as mentioned, oil glands lean more on type 1). Data currently suggests that finasteride doesn't often meaningfully lower sebum output, which makes it much less likely to improve SD via "less oil". That's the best human data I was able to find in this regard.
Dutasteride: blocks both type 1 and type 2 forms of 5-alpha reductase. It also targets the "skin/oil gland", type 1 isoenzyme. So, in theory it's a more logical option than finasteride, mechanistically, when it comes to sebaceous gland activity. That being said, do keep in mind SD isn't only an "oil problem", it's a mix of Malassezia, inflammation, as well as any person's individual sensitivity. Although dutasteride reduces scalp DHT more broadly and sounds like a better choice for us, we unfortunately still don't have strong enough evidence that it improves SD specifically, and the benefits remain theoretical/uncertain rather than proven.
https://pubmed.ncbi.nlm.nih.gov/8381804/
https://pmc.ncbi.nlm.nih.gov/articles/PMC5023004/
https://pmc.ncbi.nlm.nih.gov/articles/PMC2923939/
Minoxidil (topical):
Topical minoxidil can make SD look worse in some people: a study shows that among 400 patients using topical minoxidil for androgenic alopecia, scalp side effects included itching, increased dandruff, redness, and they say the main causes behind those symptoms are irritant contact dermatitis, allergic contact dermatitis, or an exacerbation of seborrheic dermatitis. An important note is they mention that these reactions often come from the propylene glycol rather than minoxidil itself.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10149432
Thanks for reading!
This is my first higher quality contribution to the community. I hope this will come in handy to anyone affected by this or even dandruff in the future. Open to any new ideas and/or corrections, just reply below, thank you.
If you’re dealing with SD, feel free to DM me for any questions.
Huge efforts by @Nexom for the collaboration on this thread, thanks!
Also thanks to @chadisbeingmade for checking it out as well.
This is for educational purposes only, not medical advice. A lot of what I'll be sharing in this thread comes from years of personal experience dealing with seborrheic dermatitis. Everyone's different, so results may vary (I've tried to include everything in hope that most people will yield good results). Some approaches depending on your condition can carry risks, so please just use common sense and consider talking to a professional.
Table of Contents
1. What is Seborrheic Dermatitis?
2. Why I am making this thread
3. Why does this matter?
4. Hairloss / Balding
5. The Protocol Itself
2. Why I am making this thread
3. Why does this matter?
4. Hairloss / Balding
5. The Protocol Itself
5.1 Required items
5.2 Routine
6. Interactions with environment6.1 Winter/Cold
6.2 Air Pollution
6.3 Diet
7. Interactions with other things7.1 Isotretinoin
7.2 Finasteride
7.3 Dutasteride
7.4 Minoxidil
What is Seborrheic Dermatitis? We'll refer to it as "SD" in this thread
Seborrheic dermatitis is a very common chronic skin disorder causing red, greasy, and flaky patches on areas of the body (focusing on scalp here) that are richly supplied with oil producing glands. The scalp, face, and chest tend to be affected by this type of skin disease and studies currently believe it occurs due to a combination of the yeast on your skin (malassezia), excessive production of oil, as well as an inflammatory reaction, although it is not contagious and the exact mechanisms behind its development remain poorly understood. "Dandruff" can be viewed as the most mild form of the disease and it can appear at random times.

Why I am making this thread
I've had seborrheic dermatitis since the age of 13, and tried almost every treatment, product, and method for a few years in order to manage my SD. I was able to develop a reliable protocol that currently keeps my SD under control, and also helps mask many of its signs. The information I'm providing comes from extensive testing and researching many different treatments and products. To my knowledge, there are no other places online that provide all of the information I am providing here, all in one location. People that had interest in this subject may already be aware of many things here, but I haven't found a thread mentioning all of them in relation to SD.
My case
BEFORE
Note: These photos of me were taken after already having tried a few solutions, it was way worse.

AFTER
Note: Also underwent other procedures such as hair transplant, etc.

Note: These photos of me were taken after already having tried a few solutions, it was way worse.

AFTER
Note: Also underwent other procedures such as hair transplant, etc.

Other examples
Notice how SD can manifest itself as more flakey or as more redness, this depends on the person and multiple factors.


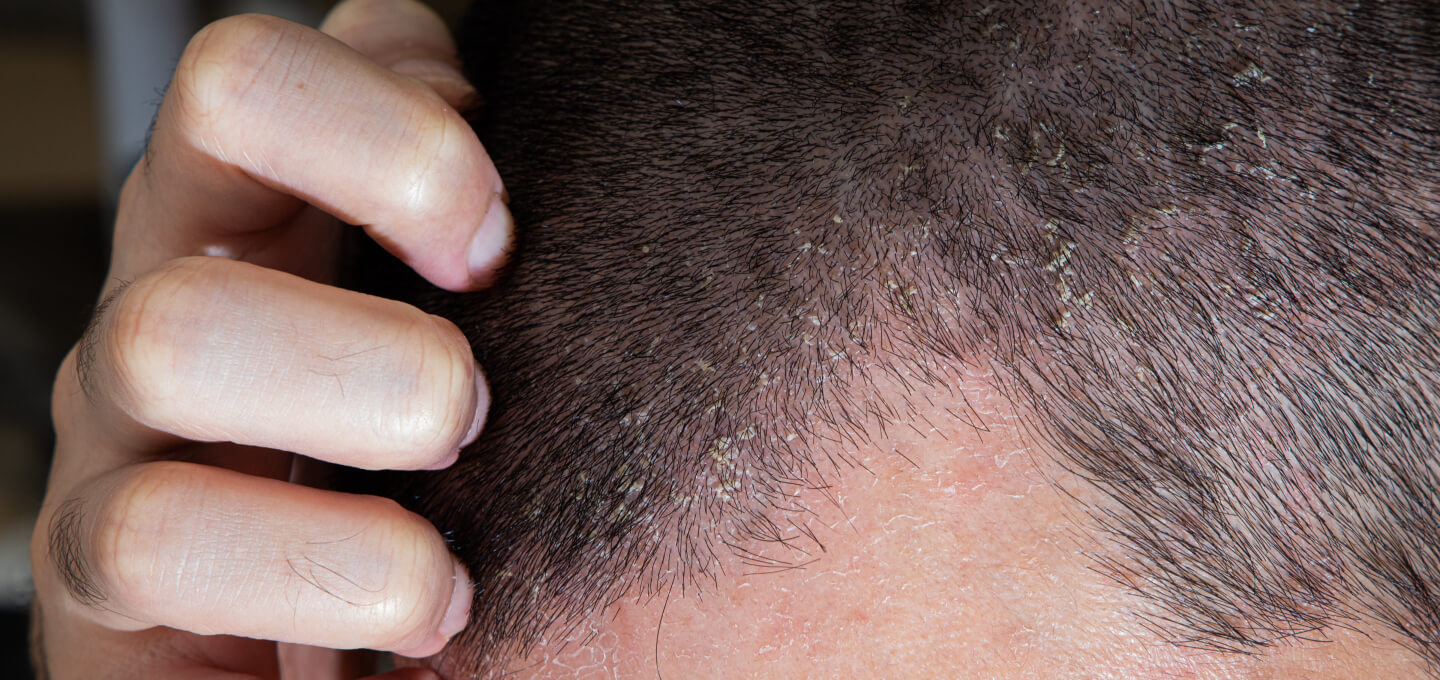
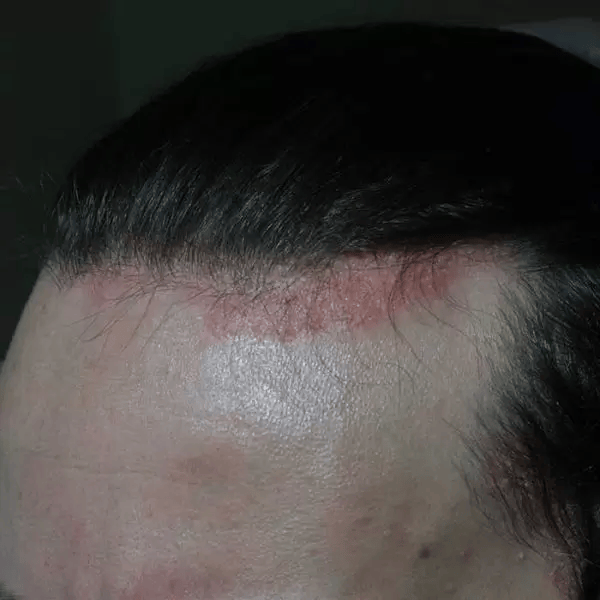
Why does this matter?
For those affected by it, SD is one of the things that barely gets talked about in looksmaxing, even though it has a big impact on how clean, healthy, and put-together you look. Flaking, redness, and weird shines can turn anyone into a subhuman and mess with how your hair looks and even skin quality. As far as I'm aware there is no "real cure". Why? Because most of it is due to: genetics, your skin barrier & how oily your skin is naturally. (https://www.ncbi.nlm.nih.gov/books/NBK551707/)
So, with the right protocol as well as by avoiding triggers and being consistent, you can keep it under control just enough for it to stop being a noticeable looksmin and burden.
Hairloss / Balding
I started balding at 17, and one factor that may have amplified it is poorly controlled SD. If you're suffering from this condition, you need to understand that once it has been active for too long, what happens is it keeps your scalp in a state of both chronic irritation and inflammation. As many of you already know from other threads, an inflamed environment in the scalp makes it more likely to create increased oxidative stress around the follicles. This can cause hairs to shed more often or even grow less strong. This basically makes thinning look worse or progress faster, on top of pre-existing genetic hair loss. This doesn't mean "SD causes permanent baldness" by itself, but it can act like an accelerator if it's left untreated. (https://pmc.ncbi.nlm.nih.gov/articles/PMC6369642/, https://pubmed.ncbi.nlm.nih.gov/16901187/)
Note: There is no STRONG evidence that this is true, we have limited observational and correlational studies.
The Protocol Itself
Required items
Nidoflor or similar variant
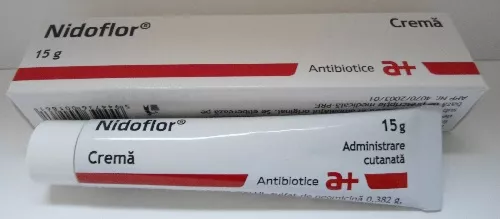
I used a product called "Nidoflor", which is a combo of triamcinolone acetonide + neomycin sulfate + nystatin (per 1g: triamcinolone acetonide 1 mg = 0.1%, neomycin sulfate 3.82mg, nystatin 100,000 IU). I haven't found this exact combo being sold anywhere else, but you could find some close matches under the form of a topical cream. (SmPC of my product in Romanian)
Here's what each of these compounds are.
Nystatin: an antifungal agent
Neomycin sulfate: a topical antibiotic
Triamcinolone acetonide: a synthetic corticosteroid
Dall'Oglio et al. (2022) report that the use of topical potent corticosteroids achieves quick control of erythema, scaling, and pruritus in seborrheic dermatitis. Just note it also warns about the risks involved.
(https://pmc.ncbi.nlm.nih.gov/articles/PMC9365318/)
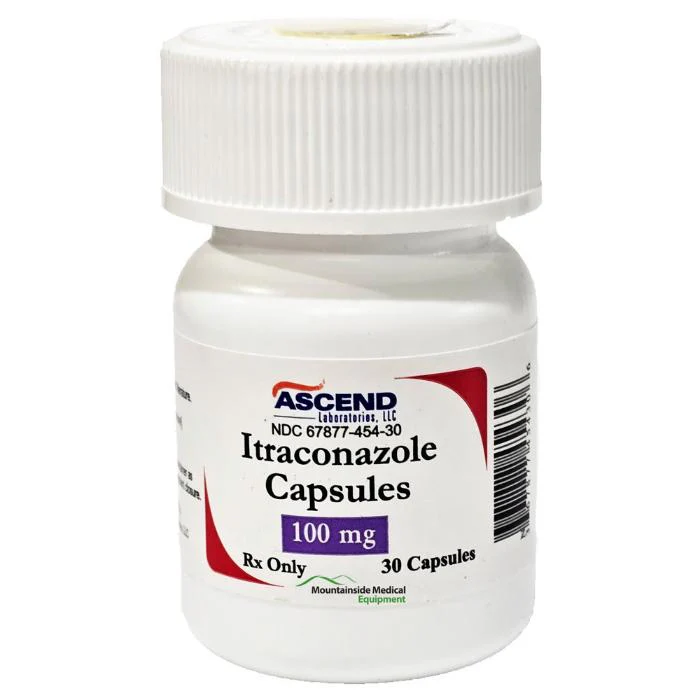
I would say this was the biggest needle mover in my case. After using itraconazole pills for just about two weeks, I had already noticed a huge reduction in the intensity of my symptoms, and after 6 weeks the symptoms were almost completely gone and I had a lot less outbreaks. Both the inflammation and scaling clearly improved from baseline. My personal observation aligns with published clinical data, where "63.4% of the patients achieve clearance of the lesions, and none had severe disease", supporting the efficacy of oral itraconazole in reducing seborrheic dermatitis severity (Nguyen et al., 2019) (https://pmc.ncbi.nlm.nih.gov/articles/PMC6364731)

Barbosa V et al. (2024) reports that prescription ketoconazole shampoo (2%) is a reliable treatment for scalp SD, and is also nicely tolerated and effective at relieving symptoms. The paper actually compares ketoconazole with selenium disulphide as an alternative but we're focusing on ketoconazole. Just note that selenium disulphide was presented as a well-tolerated alternative.
(https://pubmed.ncbi.nlm.nih.gov/39659649/)
Papavassilis C et al. (1999) reports that medium-chain triglycerides (including C8 and C10, which my MCT oil is made of) reduced the growth of Malassezia species, suggesting potential antifungal effects relevant to conditions like SD.
From my research, this study seems to be the most recent one that directly associates MCTs with growth inhibition effects on Malassezia species. There is newer research that have explored antimicrobial and antifungal properties of medium-chain fatty acids in broader contexts, but I haven't found any that directly look into the relationship between MCTs and Malassezia growth. (https://pubmed.ncbi.nlm.nih.gov/10507598/)

Optional
Cleanser


The Routine

We'll have an initial phase in which the goal is to quickly reduce scaling and inflammation and suppress Malassezia driven activity, then a maintenance phase to stop symptoms from returning. SD isn't always caused by simple fungal overgrowth. Malassezia is a normal part of everyone's skin's microbiome, and the condition is likely the result of a mix of: microbiome imbalance, barrier factors, and the individual's inflammatory response. The goal is symptom control and a more stable scalp environment, so don't consider it a permanent 'cure'.
Day 0
I strongly suggest getting a short haircut.
It helps the products reach the scalp much better and makes SD easier to manage.
First 14 days
Itraconazole:
200 mg/day for 14 days. Don't extend daily usage beyond this, as itraconazole can be hard on the liver.
MCT oil:
Apply to the most affected areas a few hours before showering, then wash it out so your hair doesn't stay greasy.
Daily shower routine:
Use lukewarm water and thoroughly soak the scalp.
Gently use the lice comb to lift/remove flakes so the shampoo can reach the scalp properly.
Apply the ketoconazole shampoo and let it sit for 5 minutes.
Rinse, then apply the shampoo one more time without letting it sit.
After the shower, pat your scalp with a towel (DON'T RUB, friction can worsen irritation).
While hair is still slightly damp, apply your variant of Nidoflor to the red + flaky areas and let it air-dry.
Nidoflor (your variant) duration:
Use it 7 days in a row only, since it contains a strong corticosteroid (and you don't want to become dependent on it)
Post 7 days
We stop using the Nidoflor (or the corticosteroid + antibiotic) but we keep showering everyday with the protocol above and keep using MCT Oil.
Post 14 days
Itraconazole:
200mg/week for 4 more weeks
At this point, we have reached the final stage. We have stopped using Nidoflor (your variant), and we will only use itraconazole once a week for a month. All that remains is to maintain our progress by following the protocol 3–4 times a week (MCT oil + ketoconazole 2% shampoo). It is highly recommended not to blow-dry your hair and instead to use a towel to remove as much moisture as possible.
Why do we keep using itraconazole?
According to the paper cited for itraconazole:
At week 2, 70% still had moderate–severe disease and only 6.7% had clearance.
At week 6, 63.4% achieved clearance.
At week 2, 70% still had moderate–severe disease and only 6.7% had clearance.
At week 6, 63.4% achieved clearance.
Interactions with environment

Winter/Cold
SD tends to be worse/more common in winter: a study shows SD showed up more often when it was colder, and it was also more common when UV/sunlight levels were lower. A simple reason is that cold weather + dry indoor heating can weaken the scalp's protective skin barrier, making it easier for irritation and inflammation to flare. Less sunlight also matters because UV light can reduce microbes (UV is used in germicidal settings to inactivate bacteria and/or fungi). This won't matter much if you're just planning on rotting indoors for the rest of your life. Anyway, the same study notes sunlight has been shown to suppress Malassezia. Lab research also found certain near-UV wavelengths can reduce Malassezia growth in a dose-dependent way (not in this specific paper). (https://pmc.ncbi.nlm.nih.gov/articles/PMC9040311/)
Solution: Shower in lukewarm water, then a apply a gentle cleanser and a moisturizer (face + hairline/scalp edges). Check if your home has dry air with a hygrometer. If it is the case then a humidifier helps, just don't overdo it. Lastly, moderate amounts of sunlight exposure can be useful.

Air Pollution
SD can also be worse in more polluted environments: a study shows people exposed to higher levels of common air pollutants had a higher risk of developing late-onset SD. That's because pollution is basically tiny particles and irritating gases that can sit on your skin and/or scalp. While this is not a huge issue, it's part of the many things that worsen SD. If you're exposed to them for a long period of time, they just become persistent mild irritants to your scalp. That can lead to inflammation, messes up your scalp's skin barrier and also ramps up oxidative stress, so you'll be losing moisture more easily. Note that there is no direct proof that this leads to SD by itself. (https://pubmed.ncbi.nlm.nih.gov/38648509/, https://pmc.ncbi.nlm.nih.gov/articles/PMC6766865/)
Solution: Use a HEPA air purifier at home (especially in the bedroom) to reduce indoor particulate pollution, which may help lower an environmental trigger.
My personal choices for air purifiers are the Airfanta 3Pro or Levoit 300S. Keep in mind this solution is not tested in this paper specifically, it's just my reasoning, common sense and hopefully a good exposure-reduction step. Lack of evidence regarding this specific solution does not mean it won't work, especially since it carries zero risk.

Diet
Based on available studies, SD seems to have a diet connection for some people, but it's not universal. One study shows that people who ate more fruit had less SD, while a more "Western" pattern (typical processed/fast-food style) was linked to more SD (fruit pattern ~ 25% lower odds, Western pattern ~ 47% higher odds). On the other hand, a case-control study reported that almost half of SD patients (49.2%) said foods did not affected their flares. In those who noticed triggers, the most common ones were sweets, spicy and fried foods, as well as dairy. Their data also showed daily bread, rice, pasta intake was more common in the SD group. The simple explanation is that lots of refined carbs can push hormones like IGF-1, and that may increase oil production and inflammation, while fruits/vegetables patterns may help via antioxidants and overall "less inflammatory" eating. (https://pmc.ncbi.nlm.nih.gov/articles/PMC10719884/, https://pubmed.ncbi.nlm.nih.gov/30130619/)
Solution: If you want to keep it simple, you've got two choices. Either do an elimination diet, or just straight up cut refined carbs/sugar (sodas, pastry, bread). Instead, try fruits and whole foods (red meat, organs, healthy fats, vegetables). This may be personal, but pasteurized dairy specifically seemed more likely to inflame me, so I just avoid that.
Interactions with other things

Isotretinoin
Isotretinoin works by shrinking the sebaceous glands. That means they make much less sebum, and with less oil, the scalp is less of a lipid-rich environment for Malassezia (lipid-dependent), and inflammation can calm. Low-dose has been studied for moderate to severe SD.
Short term: It often causes dry skin/scalp and has been shown to weaken the protective layer of the skin, which leads to moisture evaporating from the surface and triggers an irritant retinoid rash. In our case for the scalp, this shows up as more dryness, redness, itching, and flaking, especially early on.
Long term: Over months, isotretinoin can control SD symptoms while you're still taking it, but dry skin/scalp irritation can persist. Once you stop using it, SD can relapse (one study reported ~11% recurrence within 3 months). Data suggests a dose effect: 20 mg/day may provide better control and less relapses than 10 mg/day over a longer period.
https://pubmed.ncbi.nlm.nih.gov/27778328/
https://www.jaad.org/article/S0190-9622(25)02114-0/
https://www.jaad.org/article/S0190-9622(23)01351-8/
Note: I can access the JAAD papers using my student credentials, not sure if they are accessible for free.

Finasteride/Dutasteride:
Why it might help SD: My theory was that lowering DHT could reduce androgen-driven oiliness, but in practice, a human endocrine study found finasteride "did not decrease the sebum score from baseline values". That means it may not meaningfully reduce scalp oil.
Explaining type 1 and type 2
Our bodies have two main versions of 5-alpha reductase. That's the enzyme that converts testosterone to DHT, but there are better threads explaining this in detail. Simply put, type 1 is found a lot in skin/oil glands (sebaceous) and type 2 is found in tissues like hair follicles, prostate, etc. For our topic, the difference does matter, because blocking the version that's more active in oil glands is in theory more likely to affect skin/scalp oiliness.
Finasteride: mainly blocks type 2, that means, it lowers DHT in type 2 dominant tissues, but it's less likely to significantly reduce scalp sebum (as mentioned, oil glands lean more on type 1). Data currently suggests that finasteride doesn't often meaningfully lower sebum output, which makes it much less likely to improve SD via "less oil". That's the best human data I was able to find in this regard.
Dutasteride: blocks both type 1 and type 2 forms of 5-alpha reductase. It also targets the "skin/oil gland", type 1 isoenzyme. So, in theory it's a more logical option than finasteride, mechanistically, when it comes to sebaceous gland activity. That being said, do keep in mind SD isn't only an "oil problem", it's a mix of Malassezia, inflammation, as well as any person's individual sensitivity. Although dutasteride reduces scalp DHT more broadly and sounds like a better choice for us, we unfortunately still don't have strong enough evidence that it improves SD specifically, and the benefits remain theoretical/uncertain rather than proven.
https://pubmed.ncbi.nlm.nih.gov/8381804/
https://pmc.ncbi.nlm.nih.gov/articles/PMC5023004/
https://pmc.ncbi.nlm.nih.gov/articles/PMC2923939/

Minoxidil (topical):
Topical minoxidil can make SD look worse in some people: a study shows that among 400 patients using topical minoxidil for androgenic alopecia, scalp side effects included itching, increased dandruff, redness, and they say the main causes behind those symptoms are irritant contact dermatitis, allergic contact dermatitis, or an exacerbation of seborrheic dermatitis. An important note is they mention that these reactions often come from the propylene glycol rather than minoxidil itself.
https://pmc.ncbi.nlm.nih.gov/articles/PMC10149432
Thanks for reading!
This is my first higher quality contribution to the community. I hope this will come in handy to anyone affected by this or even dandruff in the future. Open to any new ideas and/or corrections, just reply below, thank you.
If you’re dealing with SD, feel free to DM me for any questions.
Huge efforts by @Nexom for the collaboration on this thread, thanks!
Also thanks to @chadisbeingmade for checking it out as well.
Last edited: