Recessed Bateman
Biohacking and dermatology
- Joined
- Dec 6, 2025
- Posts
- 515
- Reputation
- 515
Table of contents:
- Intro
- Identification/Diagnosis
- Treatment/Protocols
- Extra advice
Intro:
A face and body full of acne or folliculitis is a massive halo killer. It nukes your skin texture and ruins your "clean" look. There’s no need to justify why this guide is necessary, skin imperfections are a huge failo.

My mission here is to provide actual dermatological knowledge for those of you rotting with skin issues because your derm gave you some generic "wash your face" cope.
This guide is especially vital if you are currently on, or have finished, an Isotretinoin (Accutane) cycle.
Identification/Diagnosis
You need to know if you're fighting bacteria or a compromised skin barrier.
Treating folliculitis like regular acne will only make it worse.
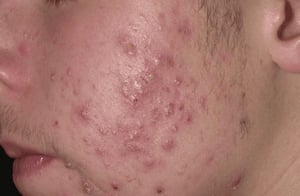
How to spot Acne (Vulgaris):
- Location: Face and Body (random spots)
- Pathology: Excess sebum + clogged pores + C. acnes colonization.
- Appearance: Comedones (blackheads/whiteheads) or inflammatory papules/pustules and cysts.
- Symptoms: Tenderness and deep, throbbing inflammation.
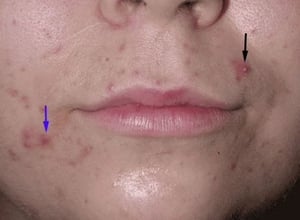
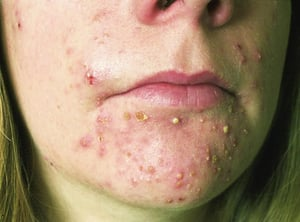
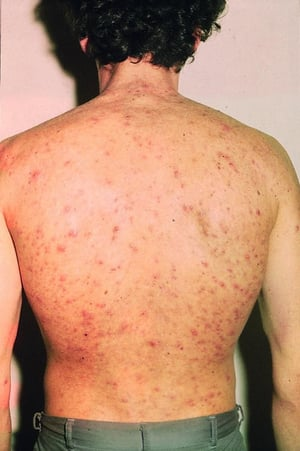
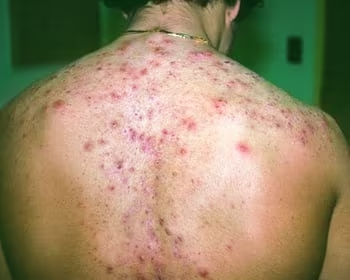
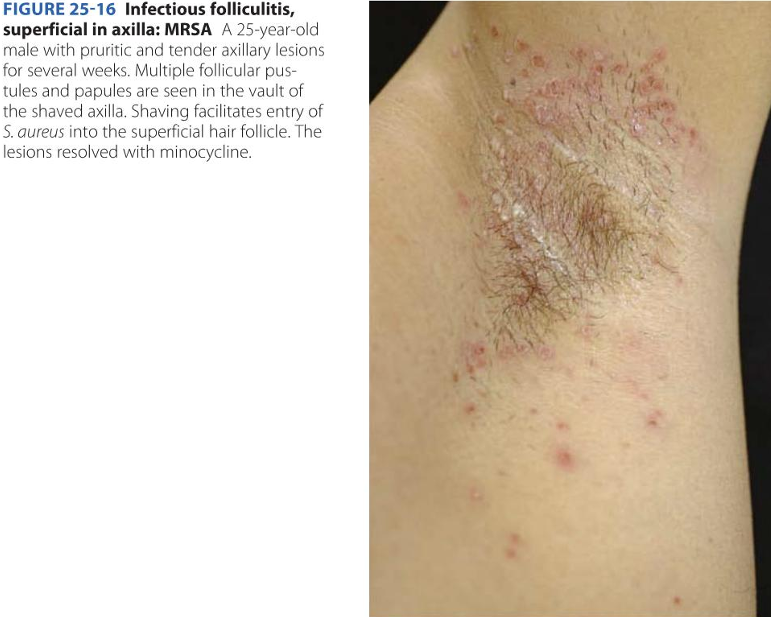
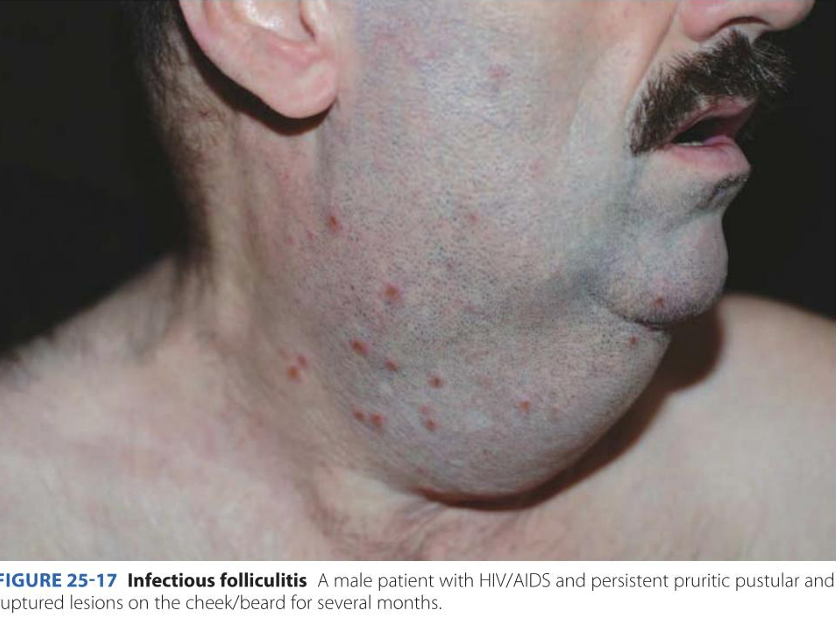
How to spot Folliculitis:
- Location: Anywhere with hair follicles. Common on the beard area (face), neck, chest, scalp, and glutes.
- Pathology: Infection of the hair follicle itself, usually by S. aureus (bacteria), viruses, or fungi.
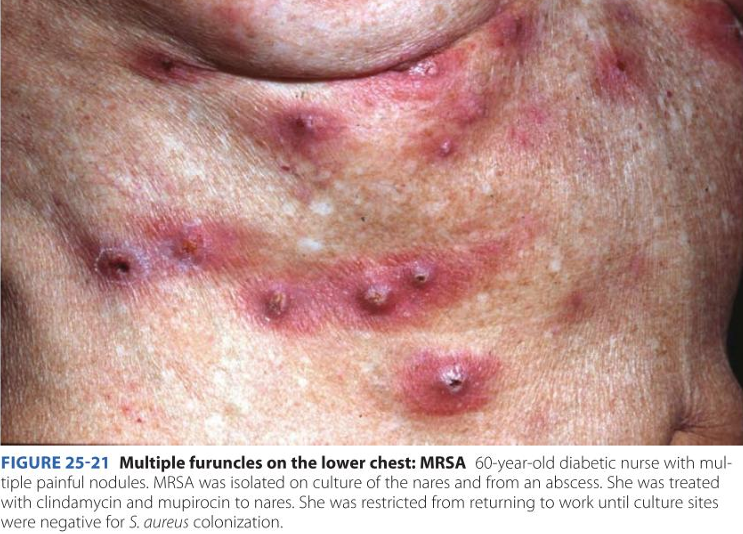
- Appearance: Small, red, itchy bumps centered around a hair. If left untreated, it progresses into a Furuncle (abscess/boil).
- Symptoms: High itchiness (pruritus) and localized discomfort. Unlike acne, it often feels "surface-level" but stings.
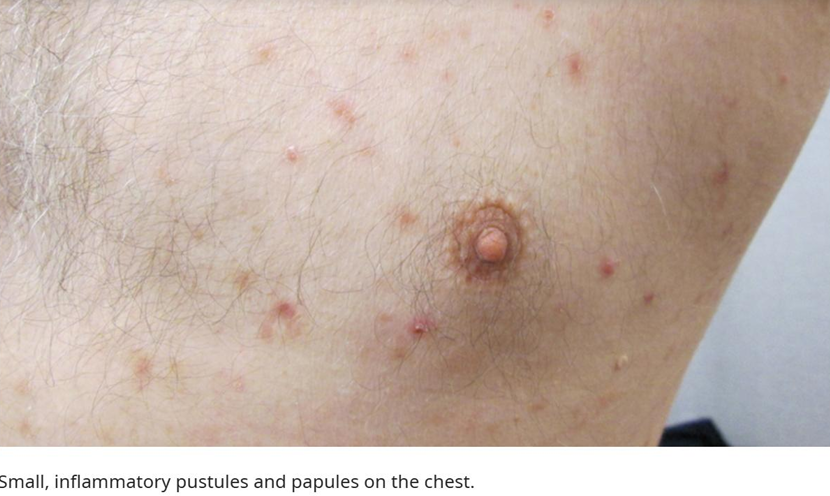

Treatment/Protocols
ACNE PROTOCOL (Face & Body)
A. Non-Accutane Users:- Hygiene: You need to de-clog the follicle. Use a cleanser with Salicylic Acid (BHA) or Benzoyl Peroxide. The goal is to nuke the keratin plug in the epidermis so sebum can flow freely.
- Infection Control: Use Topical Retinoids (Adapalene/Differin/Tretinoin) to normalize skin cell turnover, combined with local antibiotics like Erythromycin or Clindamycin
CRITICAL RULE: DON’T TOUCH IT. JUST APPLY THE RETINOIDS.
- Stop "picking" at your skin like an IQlet subhuman. Every time you squeeze a cyst, you’re pushing the infection deeper and guaranteeing a permanent scar.
For active cystic breakouts or stubborn spots, I highly recommend Epiduo Forte (Adapalene 0.3% + Benzoyl Peroxide 2.5%).
- Why it works: It’s a 2-in-1 combo. The Adapalene forces cell turnover while the Benzoyl Peroxide oxygenates the pore, killing C. acnes instantly.
Unlike topical antibiotics, bacteria can't develop resistance to BPO. - Protocol: Use it as a spot treatment.

- Fail-safe: If it doesn’t improve, suspect Malassezia Folliculitis (fungal acne) which feeds on lipids. If you're on a cycle (PEDs) or nothing works, stop wasting time and hop on oral Isotretinoin.
B. On-Accutane Protocol:- Check this guide for the basics:
[the ultimate accutane isotretinoin guide - @pentaChad_doomer ] - Mechanism: Isotretinoin nukes sebum production. No sebum = no food for C. acnes.
- Requirement: Intensive heavy-duty moisturizers to combat Xerosis (extreme dryness).
FOLLICULITIS PROTOCOL (Face & Body)
A. Non-Accutane Users:- Hygiene: Use an antibacterial wash (e.g., Chlorhexidine or Hibiclens).
- Infection Control: Since S. aureus is the usual culprit, use Mupirocin or Clindamycin ointment.
- Note: If no progress is made, it might be Pseudomonas or Fungal. Large furuncles may require surgical drainage.
B. On-Accutane Protocol (Crucial):
On Accutane, your epidermis becomes paper-thin. This creates micro-fissures. Bacteria (S. aureus) that usually live harmlessly on your skin enter these cracks and cause folliculitis. This is not "oily" folliculitis; it’s "broken barrier" folliculitis.
- Hygiene: STOP using harsh antibacterial soaps or scrubs. Switch to a Syndet (Soap-free) cleanser (e.g., La Roche-Posay Lipikar Gel or CeraVe Hydrating).
- Treatment: Targeted Mupirocin or Clindamycin for the S. aureus.
- Water Control: Hot water = vasodilation = more itching and inflammation. Use lukewarm water and pat dry; never rub your face or body with a towel.
- Barrier Restoration: Apply an emollient (e.g., Lipikar Baume AP+M) immediately post-shower. If you don't, TEWL (Transepidermal Water Loss) will happen, making it easier for bacteria to penetrate.
Extra advice
- GHK-Cu (Sub-Q): Highly recommended if you are on Accutane. It helps thicken the skin barrier and speeds up scar healing (Accutane slows it down). It prevents that "sunken/thin skin" look, especially in the under-eye area.
[Check these guides: how to properly use ghk-cu - @NZb6Air , you cant use ghk cu with bac use pbs - @SlayerJonas ] - KPV Peptide: Great for nuking systemic inflammation and has mild antimicrobial properties. Helps with persistent redness.
- Oral supplements for Accutane users:
- Omega-3: Essential for joint lubrication and skin lipids.
- Vitamin B5 (Pantothenic Acid): Helps with skin repair.
- Liver Support: NAC + ALA to keep your enzymes in check.

Sourcing
GHK-CU and KPV sourcing guides:
A. Grey market option:
Go through this website https://glp1forum.com/
Scroll down and you will see a list of vendor sources.
Guide on how to find sources yourself:
[you need to find sources yourself and eviscerating jallrd - @aids ]
B. Search in google option:
I have bought from Kensingtonlabs, Semaxpolska, XLpeptides (Europe sources)
Attachments
Last edited: