81xa
135 IQ
- Joined
- Sep 21, 2023
- Posts
- 1,527
- Reputation
- 1,900
Hormones
This guide breaks down 30+ hormones, including Growth Hormone, Prolactin, Oxytocin, CCK, and more. Instead of me just telling you what to do, each section walks through the actual mechanisms and pathways so you understand the reasoning behind everything. By the time you finish reading this, you'll know how these hormones shape your body on a daily basis and how to work them in your favour.
When a hormone gets referenced inside another hormone's section, the full explanation is in that hormone's dedicated section. If I mention "lower serotonin" while covering prolactin, the how-to is in the serotonin section.
Note on Sources: Numbers in brackets throughout the guide are PMIDs. Plug them into PubMed and you'll find the study directly. Don't take my word for it, read the research yourself.
Every micronutrient that comes up, quercetin, taurine, apigenin, magnesium, vitamins C, E, A, and the rest, is covered in a nutrition reference section at the end. It lists the best food sources and notes where supplementation is a viable option.
What Are Hormones?
Hormones are chemical messengers the body uses to coordinate specific processes. They're molecules released into the bloodstream, mostly by the endocrine system, glands like the testicles, adrenals, thyroid, and pituitary.They interact with other hormones, which then influence other processes downstream.
- Antagonistic: When two hormones have opposite functions or suppress each other. Dopamine and prolactin are antagonistic; dopamine directly suppresses prolactin, and prolactin directly suppresses dopamine.
- Agonistic: When two hormones activate each other. Prolactin and estrogen are agonistic; prolactin amplifies estrogen receptor sensitivity.
That's what makes them master regulators, arguably the most impactful molecules in your body.
Most people have multiple hormones out of balance at any given time. They're all interconnected. When one is off, it pulls others with it.
Prolactin
Prolactin is produced by lactotrophs in the anterior pituitary. It's primarily a female hormone; its main job is stimulating breast milk production during pregnancy. Prolactin receptors exist across the entire body, which means chronically high levels create widespread damage.Effects of High Prolactin:
- Lowers testosterone (2823160)
- Lowers LH
- Lowers GnRH (9506732)
- Reduces LH receptor sensitivity in the testes
- Lowers dopamine
- Inhibits bone formation (10718830)
- Stimulates bone resorption (6490793)
- Causes erectile dysfunction (31044754)
- Makes tissue more sensitive to estrogen (gynecomastia)
- Stimulates nipple lactation
- Reduces androgen receptor sensitivity
- Makes you passive (1576086)
- Lowers DHT (2943108)
The issue is most of us live in a way that chronically spikes prolactin
Things That Raise Prolactin:
- Low dopamine (8284103)
- Alcohol (7375492)
- High cortisol (3067562)
- Serotonin and SSRIs (4060968)
- High estrogen
- Weed
- Masturbation
- Low calcium intake
- Oxytocin
- TRH (Thyrotropin releasing hormone)
- Hypothyroidism
- High body fat / high leptin
- Sauna
- Tryptophan
The Average Modern Male: 20%+ body fat, hours of TikTok daily, masturbates, drinks on weekends, smokes weed, sleeps badly, and has poor T4 to T3 conversion. Every single one of those things raises prolactin.
Dopamine
Dopamine directly antagonises prolactin. More dopamine means less prolactin. Here's how to maximise it from the ground up.Dopamine Synthesis
1. L-Phenylalanine
The body can't produce phenylalanine, it has to come from food. Best sources: meat, dairy, eggs. The enzyme that converts phenylalanine into tyrosine is Phenylalanine hydroxylase (PAH). To keep it running properly:- Lower oxidative stress
- Iron (from meat)
- Vitamin C
- NADPH (via B3, magnesium, and thiamine, for BH4 cofactor activity)
2. L-Tyrosine
The body can make tyrosine, but diet is the most reliable way to raise it. Best sources: meat, eggs, dairy, fish. Tyrosine converts into L-DOPA via tyrosine hydroxylase. To boost this enzyme:- Vitamins B2, B3, B9
- Vitamin C and E
- NAC
- Antioxidants
- Bromantane
3. L-DOPA
The final step before dopamine. To raise L-DOPA: high protein diet, L-tyrosine supplementation, B vitamins, vitamin C. The enzyme converting L-DOPA to dopamine is AADC (Aromatic L-amino acid decarboxylase). Required nutrients:- Vitamin B6
- Magnesium
- Zinc
- Vitamin B3
Dopamine Receptor Sensitivity
All the dopamine in the world does nothing if your D2 receptors are desensitised.What kills D2 receptor sensitivity:
- Porn
- Gaming
- Gambling
- Junk food
- Doom scrolling
How to restore receptor sensitivity:
- Morning sunlight
- B vitamins and vitamin C
- A consistent circadian rhythm
- Lowering stress
- Long-term goal pursuit, working hard, reading, building skills
The Dopamine Detox: Removes all unnatural dopamine spikes and gives the brain time to upregulate receptors properly. This accelerates recovery if you've seriously damaged your receptors:
- No screens
- No music
- No caffeine or nicotine
- 10 hours of sleep
- Time in nature
- Food focused on dopamine synthesis
Other Ways to Lower Prolactin
- Lower serotonin
- High calcium intake (low calcium raises PTH, which stimulates prolactin)
- Healthy thyroid (hypothyroidism raises TRH, which directly stimulates prolactin)
- Better sleep quality (high cortisol raises prolactin)
- P5P
- Thiamine
- Royal Jelly
- Pramipexole
- Dopamine agonists
- Lower estrogen
- Vitamin E
- Vitamin A
- Less tryptophan during the day
- Aspirin
Serotonin
Serotonin (5-HT / 5-hydroxytryptamine) is technically a neurotransmitter, not a hormone. But its effects are so hormone-like, and it gets referenced so often throughout this guide, that it needs its own section.Low serotonin is better than high serotonin. The body has it for a reason, but the negative effects are consistently ignored in mainstream health content.
Serotonin gets praised as the "happy hormone" and the supposed cure for depression. The evidence doesn't support that. Large numbers of depressed people have no serotonin deficiency and still get prescribed SSRIs. (35854107) There are drugs that increase serotonin reuptake, the opposite mechanism to SSRIs, that outperform SSRIs at treating depression. (11463130)
Postmortem studies on suicide victims show overexpressed 5-HT2C receptors. Systematic reviews of randomised clinical trials link SSRIs to higher suicide attempt rates. (15718539, 11988167)
Elevated Serotonin Causes:
- Slowed metabolism (7875554)
- Lower heart rate and body temperature (15802554)
- Reduced ATP production, disrupts mitochondrial electron transport chain complexes 1-3 (1759390)
- Diarrhoea (1691117)
- Passivity and withdrawal under pressure (19423206)
- Laziness
- Increased prolactin
- Aggression (35257831)
- Anxiety
- Sexual dysfunction (73% of SSRI users report it)
- Cognitive impairment
- Higher suicide attempt rate
- Increased bone resorption (27581523)
- Decreased bone formation via 5-HT6R / BMP-2
- Lower testosterone
- Lower sperm quality (40371979)
- Stunted GH release
- Reduced T3
- Increased inflammation (1581411)
- Increased aromatase activity (28442777)
High-Serotonin Foods to Limit:
Turkey, chicken, ashwagandha (37878284, 30854916), soy, pumpkin seeds, almonds, cashews, bananas, pineapple, eggs, beef, salmon, tuna, sardines.Some of these are healthy foods. The point isn't to eliminate them, it's to be conscious of intake and limit them where needed. Soy and seed oils are the exception. Avoid those entirely.
When to Eat Serotonin-Raising Foods Strategically:
Serotonin is a precursor to melatonin. The process:- Serotonin
- N-acetylserotonin (via AANAT)
- Melatonin (via HIOMT)
Swap in collagenous foods:
- Gelatin powder
- Meat on the bone
- Skin-on meat
- Bone broth
- Oxtail soup
Hormones That Affect Serotonin
- Increase serotonergic activity: Estrogen, prolactin, cortisol, leptin
- Decrease serotonergic activity: T3, T4, testosterone, ghrelin, progesterone
Monoamine Oxidase (MAO)
MAO is the enzyme that breaks down and metabolises neurotransmitters.Two forms: MAO-A and MAO-B.
- MAO-A metabolises: Serotonin, adrenaline, noradrenaline, dopamine (partially), melatonin (partially)
IMPORTANT WARNING: Do not inhibit MAO while taking serotonergic compounds (SSRIs, ashwagandha, etc.). This combination causes serotonin syndrome. It can seriously harm you.
- Things that increase MAO-A: Vitamin B2, low estrogen, valproic acid, good circadian rhythm, thyroid health
- Things that decrease MAO-A (do not combine with serotonergic compounds): Methylene blue, quercetin, EGCG, resveratrol, ayahuasca, linezolid, garlic, saffron, passionflower tea, fenugreek, smoking, coffee, high estrogen
Lowering Serotonin via the Gut
90-95% of the body's serotonin is produced in the gut by enterochromaffin cells. This is why serotonin-targeting drugs have such strong digestive effects.Examples:
- Mirtazapine: Antidepressant that sharply increases food intake via 5-HT antagonism
- Zofran: Prevents nausea and vomiting in chemo patients
- Prucalopride: Treats constipation via gut motility
- Tropisetron: Used in IBS
Keeping Gut Serotonin in Check:
- Ray Peat's carrot salad (raw carrot, coconut oil, ACV, salt)
- Potatoes
- More calcium
- Better T3 production
- Fewer beans and lentils
- Pair carbs with protein or fat
- Less junk food (SCFAs raise 5-HT)
- Whole foods
- Ginger tea
- Antioxidants
- Active lifestyle (movement prevents gut fermentation)
- Mushrooms
- Oral hygiene
- Probiotics
Other Ways to Lower Serotonin
- Diet: Less tryptophan, more LNAAs (glycine, tyrosine, leucine compete with tryptophan at the blood-brain barrier), avoid whey / alpha-lactalbumin, sodium, magnesium, L-theanine, thiamine, L-lysine, glycine, taurine, ginger, vitamin E, no seed oils
- Lifestyle: HIIT over endurance, lower prolactin, lower estrogen, raise testosterone (increases SERT, which reuptakes serotonin), raise melatonin, aspirin, eat smaller meals regularly
Dopamine, Serotonin & Prolactin
(Theory only)Dopamine is excitatory. The body uses several mechanisms to inhibit it: COMT, MAO, GABA, and serotonin.
Serotonin is a potent inhibitor of tonic dopamine. Dopamine is what creates drive, motivation, and forward momentum. Serotonin blunts that. This is not something to promote.
Serotonin also increases prolactin by stimulating the pituitary via 5-HT2, further suppressing dopamine and androgenic drive.
Learned Helplessness
Serotonin blunts the learning response and produces learned helplessness, the state where challenge feels uncontrollable and effort feels pointless. You stop trying new things. You go with the flow.Mechanism:
- Stressors activate the dorsal raphe nuclei, releasing serotonin broadly.
- Activation of 5-HT2C receptors in the striatum and prefrontal circuits reduces dopamine neuron activity.
- This suppresses the reward-prediction error signal.
- Over time, this builds into a baseline of high prolactin, lower testosterone, and slower thyroid function.
The body also adapts over time. If every surge of dopamine and androgens gets consistently met with inhibition from prolactin, serotonin, and cortisol, the brain learns not to attempt excitation. Androgen and dopamine receptors downregulate. The body stops trying.
Estrogen
Estrogen is actually a group name. The active form in men is estradiol (E2). Estrone (E1) has roughly 10% of E2's potency. Estriol (E3) is negligible. Focus on E2.Estrogen is 30-60% bound to SHBG and acts through two distinct receptors:
- ERα: Sexual health, bone density, fat storage, insulin sensitivity, vascular health, aggression in men, growth plate closure
- ERβ: Neuroprotection, insulin sensitivity, immune function, anxiolytic effects, stress reduction
Estrogen is primarily produced through the aromatase enzyme, which converts testosterone into estradiol. Aromatase is densely concentrated in fat tissue. A small amount of estrogen is also made directly by the Leydig cells in the testes.
Effects of High E2:
- High fat mass
- Insulin resistance
- Fatigue
- Sexual dysfunction
- Low drive
- Passive aggression
- Chronic stress
Hormone Crosstalk With Estrogen
- Prolactin: E2 binds to estrogen receptors on lactotroph cells in the pituitary, activating prolactin transcription. Prolactin in turn increases ER sensitivity, which is how gynecomastia develops in men. High estrogen also blocks dopamine's ability to suppress prolactin (by weakening D2 signalling), which creates a self-reinforcing prolactin-estrogen cycle. E2 also stimulates lactotroph proliferation; more lactotrophs means more prolactin.
- Serotonin: E2 decreases MAO-A activity, leaving serotonin to accumulate. It increases TPH2 (serotonin synthesis) and reduces SERT, the reuptake transporter SSRIs target. Estrogen essentially acts as a weak endogenous SSRI. It also lowers 5-HT1A, which normally brakes serotonergic activity, resulting in more 5-HT overall.
- Oxytocin: E2 increases oxytocin gene transcription, upregulates oxytocin receptors, and increases oxytocin receptor density in the brain.
- Cortisol: Estrogen blocks the negative feedback loop that normally shuts off cortisol, leading to more cortisol release. It upregulates HPA axis activity and CRH expression (CRH → ACTH → cortisol), and reduces GABA, which would otherwise keep the HPA axis in check.
- Testosterone: E2 binds to estrogen receptors on the hypothalamus, suppressing GnRH and interrupting testosterone production at the start of the cycle. Enclomiphene works by blocking exactly this feedback.
How to Lower Estrogen
Optimal E2 range for men: 20-35 pg/mLAvoid pharmaceutical aromatase inhibitors if you're under 25. They're difficult to control and can create more problems than they solve. Natural methods are more than sufficient.
- Hormones that naturally lower aromatase: DHT (can't be aromatised), progesterone, melatonin, T3, T4
- Lowering aromatase expression: No alcohol, lower HIF-1α (build CO2 tolerance), lose excess fat (12% body fat is optimal for most), chrysin, naringin, quercetin, apigenin, liver (food), vitamin A, resveratrol, lower cortisol, lower prolactin, improve insulin sensitivity, pomegranate juice, melatonin, nettle tea, vitamin E
- Promoting estrogen clearance: E2 is deactivated by the liver. The following impair that process: fatty liver, hypothyroidism, nutrient deficiencies (folate, B12, B6), high homocysteine (slows COMT), heavy metals, alcohol, oxidative stress, low fibre. To support clearance: DIM, IC3, raw carrots, calcium D-glucarate, Lactobacillus probiotics, exercise
- Lowering inflammation: Lower cortisol, vitamin C, vitamin E, vitamin D, magnesium, sleep, fruit, no PUFAs, polyphenols, glutathione, NAC, glycine, taurine, some L-glutamine, aspirin
Estrogen Relationships
- Estrogen and GH/IGF-1: Balanced E2 is actually beneficial for GH. It inhibits somatostatin, the primary brake on GH secretion. Men with a genetic aromatase deficiency show low IGF-1 levels as a likely consequence. For naturals: do not take an AI thinking it will make you taller. It won't.
- Testosterone and Estrogen: Testosterone makes men assertive. Estrogen makes men aggressive. Uncontrolled rage is an imbalance between T and E2, not high testosterone on its own.
- Estrogen and Height: Estrogen is the primary driver of growth plate closure. The mechanism: local aromatisation of testosterone into E2 → E2 binds ERα → triggers closure pathways. DHT cannot aromatise. Combined with low systemic E2 and low aromatase expression, you get the most favourable conditions for keeping plates open as long as possible.
Growth Hormone
GH is one of the most important hormones for height, bone growth, muscle building, and body composition.How GH works:
- GH binds to the GH receptor.
- Recruits JAK2, which phosphorylates and activates the receptor.
- This recruits STAT5, which drives transcription of IGF-1 and other targets.
- GH also activates MAPK/ERK (cell proliferation and differentiation) and PI3K/AKT (metabolic and cell survival) pathways.
GH is secreted in 8-10 pulses per 24 hours in men, mostly during deep sleep. The first 1-2 pulses in the first two hours of sleep account for up to 65% of total daily GH output. Sleeping slightly shorter than usual is less damaging than most people think.
Main Functions of GH:
- Shifts the body into fat-burning mode
- Directly stimulates bone growth and chondrocyte proliferation
- Reduces muscle glucose uptake (IGF-1 counteracts this)
- Increases protein synthesis
- Increases collagen synthesis (so significantly that collagen turnover testing is used in doping tests)
- Increases liver glucose output
- Supports wound healing via fibroblast and keratinocyte proliferation
- Causes fluid retention through sodium reabsorption
How GH Interacts with Other Hormones
- Cortisol/HPA: Acute stress can spike both cortisol and GH. Chronic stress suppresses both. High cortisol inhibits GH and reduces post-receptor transcription.
- Thyroid: GH and thyroid hormones reinforce each other's effects on growth. GH can also increase T4-to-T3 conversion.
- Testosterone/Estrogen: Estrogen is crucial for GH pulsatility and potency. Testosterone supports GH primarily through conversion to E2.
- Prolactin: GH and prolactin are evolutionarily related and can bind each other's receptors at high concentrations. This is why very high GH can produce prolactin-like side effects.
- Neurotransmitters: GABA raises GH by increasing deep sleep and through direct action at the pituitary. Ghrelin (the hunger hormone) is a powerful GH stimulant.
Maximising GH
- Lifestyle: High-intensity exercise (sprints, heavy lifting), avoid endurance training, manage stress, red light therapy (670nm), avoid snacking, optimise thyroid, prioritise deep sleep, stay active throughout the day
- Sleep support: Magnesium bisglycinate, L-theanine, taurine, valerian root, lemon balm, glycine
- Diet: High protein, no high-carb meals 2-3 hours before bed (spikes insulin which suppresses GH), gelatin, vitamin A, lysine, arginine, ornithine, glycine, leucine, medium-to-high fat intake, caffeine (timed appropriately), no alcohol
- Supplements: Zinc and copper, creatine
- Pharmaceuticals: Ipamorelin + CJC DAC (maximises GH spikes and pulsatility without receptor desensitisation), MK-677 (effective but raises prolactin and hunger), GH itself (most effective, most expensive)
- Best pharmaceutical sleep optimisers: daridorexant, lemborexant, trazodone
GH to IGF-1 Conversion
GH is converted to IGF-1 in the liver via the JAK2-STAT5 pathway. To maximise systemic IGF-1, the liver has to be functioning at a high level. Here's every step of the conversion process and what it needs:- Step 1: GH binds to GHR, activates JAK2 → phosphorylates STAT5. Required nutrients: magnesium, selenium, iodine, cholesterol, zinc, vitamin A, carbs
- Step 2: STAT5b enters the nucleus and switches on the IGF-1 gene. Required nutrients: vitamins B5, B6, B9, B12, choline, betaine, methionine
- Step 3: IGF-1 gene is transcribed and translated into protein via mTORC1. Required nutrients: leucine (mTOR), arginine (mTOR), magnesium, potassium
- Step 4: IGF-1 is processed from its precursor form into the final 70 amino acid hormone. Required nutrients: vitamin B2, cysteine, glutathione, calcium
Things That Impair GH-to-IGF-1 Conversion:
- Fasting (raises SOCS, FGF21, SIRT1, all inhibit JAK2)
- Low calorie diets
- Inflammation
- SARMs or oral steroids without managing liver impact
- Visceral fat
- Fatty liver disease
- Iron overload (from too much red meat or iron + vitamin C stacked together)
- Liver-damaging supplements (ashwagandha, accutane, etc.)
Liver Health Protocol
The liver handles E2 clearance, T3 conversion, and IGF-1 production. It deserves serious attention. Pick the options that fit your situation:1.5g protein per kg bodyweight, glycine, taurine, choline, no PUFAs, no seed oils, adequate carbs, 12-hour eating window, coffee, zinc, vitamins D/A/E, selenium, 2-4L fluids daily, no alcohol, TUDCA, orange juice, low-dose aspirin, saturated fat, antioxidants, magnesium, NAC, CoQ10, royal jelly, pomegranate juice, boron, green tea, milk thistle, gelatin or collagen to balance amino acids, Ray Peat carrot salad (raw grated carrot, coconut oil, salt).
A Note on Organ Acromegaly: Maximising GH naturally will not cause organ acromegaly. Chronically supraphysiological IGF-1, from multi-year, high-dose GH injections, is the actual cause. Following everything in this guide puts you at the upper end of normal ranges, not into acromegaly territory.
Dihydrotestosterone (DHT)
DHT is converted from testosterone by the enzyme 5-alpha-reductase, which comes in three forms. Only 5-AR I and 5-AR II are relevant here.Critically: DHT conversion happens locally in tissues like the scalp, prostate, and skin. Blood DHT levels are a poor indicator of what's actually happening in those tissues.
- 5-AR I: Primarily expressed in skin, scalp, brain, liver, and to a lesser extent the prostate. Dutasteride inhibits this more effectively than finasteride.
- 5-AR II: Primarily expressed in the prostate, penis, and scalp. Major driver of masculine characteristics and sexual dimorphism.
What DHT Actually Does
- Development: Masculinisation, development of sexual characteristics, modulation of NOS and PDE5 in the penis (same mechanism as Viagra), facial and body hair, sebum production.
- Muscle: DHT promotes mTOR signalling, satellite cell differentiation, protein synthesis, and genomic AR signalling. On its own it's not a primary hypertrophy driver, but it can amplify hypertrophic signalling, especially at higher levels.
- Bone and Height: Growth plates express 5-AR, allowing local testosterone conversion to DHT. DHT drives chondrocyte proliferation via potent AR activation, increases matrix synthesis, and promotes periosteal bone expansion, producing wider, stronger bones.
- Full positive effects of testosterone on growth plates
- Amplified effects via potent AR activation
- No estrogen-driven plate closure
Metabolites: 3α-diol and 3β-diol
DHT converts into these two metabolites via 3α-HSD and 3β-HSD. They're the reason DHT has cognitive and neurological benefits.- 3α-diol: GABA-A positive allosteric modulator, increases inhibitory activity, raises stress tolerance, lowers anxiety, improves slow-wave sleep (important for GH secretion), enhances cognitive function, promotes calmness.
- 3β-diol: ERβ agonist, anti-inflammatory in the brain, neuroprotective, dampens HPA axis, reduces stress.
Increasing DHT
- To Raise: Testosterone, zinc, creatine (15-25g), boron, butea superba, sunlight (vitamin D3), magnesium, moderate-to-high fat diet, cholesterol, nutrient-dense diet, 1.5g+ protein per kg bodyweight, coffee, healthy body fat percentage, sprints, competition, low stress, confidence (DHT and confidence form a positive feedback loop), thyroid health, glycine, taurine, ginger, gelatin, MCT oil, HCG, DHEA.
- What Lowers DHT: Prolactin, soy, estrogen, PUFAs, alcohol, cortisol, chronic inflammation, micronutrient deficiencies, hypothyroidism, BPA and endocrine-disrupting chemicals.
DHT and Other Systems
- SHBG: DHT has high affinity for SHBG and also suppresses SHBG synthesis in the liver, reducing bound hormone levels.
- Cortisol/HPA: DHT and 3β-diol suppress CRH, reducing cortisol. High cortisol states suppress DHT by reducing gonadotropins and 5-AR activity.
- Thyroid: Hyperthyroidism raises SHBG, lowering free DHT. Hypothyroidism lowers SHBG. Thyroid hormones regulate 5-AR expression in both directions.
- GH/IGF-1: Higher GH increases 5-AR activity and DHT metabolites. DHT works synergistically with IGF-1.
- Insulin: Insulin stimulates steroidogenesis and hepatic 5-AR, increasing DHT.
- Neurotransmitters: 3α-diol potentiates GABA-A, increases dopaminergic activity, and increases serotonin reuptake (lowering 5-HT). 3β-diol activates ERβ, supporting reward circuits and sexual arousal. DHT is severely underrated for mental function and drive.
DHT and Hair Loss
Normal DHT levels do not cause hair loss. DHT amplifies hair loss in a specific, already-broken environment; it is not the root cause.Here's the actual environment of a balding scalp:
Balding scalps show a dysfunctional mitochondrial electron transport chain; ATP production drops sharply in affected areas (35119146). Blood flow is impaired specifically in balding zones, not elsewhere (2715645). Low oxygen (hypoxia) in the follicle is pro-hair loss. HIF-1α and NADPH, which help cells survive low-oxygen states by shifting to glycolytic energy production, are abnormally low in balding scalps.
Minoxidil works by increasing blood flow to the scalp and stabilising HIF-1α, allowing glycolysis to resume. But it doesn't fix the underlying environment, which is why hair falls out again when you stop.
DHT in this environment amplifies follicle damage. That's why 5-AR inhibitors slow hair loss; they remove an amplifier. They do nothing about the actual problem: mitochondrial dysfunction, low blood flow, oxidative stress, and inflammation.
Summary:Note: Testosterone and DHT both decline with age, while hair loss accelerates. If DHT were the root cause, the pattern would run the opposite way.
- DHT is an amplifier in a damaged environment, not the root cause.
- The environment is: low blood flow, low oxygen, mitochondrial ETC dysfunction, low ATP, high oxidative stress and inflammation.
- HIF-1α and NADPH are low; glycolysis is impaired; follicles enter an energy crisis.
- DHT amplifies damage in that state.
- 5-AR inhibitors remove the amplifier but leave the cause untouched.
DHT in the Brain
DHT enhances neuron survival and increases GABA activity. People who take 5-AR inhibitors often become highly stressed despite elevated testosterone, because it's DHT, not testosterone, that keeps the brain calm.It supports mood regulation and learning efficiency, and is associated with reduced risk of neurodegenerative diseases including Parkinson's and Alzheimer's.
Triiodothyronine (T3)
T3 is the active thyroid hormone. It regulates metabolism, cellular energy production, and dozens of downstream processes. It's also one of the most important hormones for physical appearance.What T3 regulates: Thermogenesis, macronutrient metabolism, metabolic enzymes, cardiovascular function, development, and the cortisol/testosterone/DHT/GH-IGF-1 axis.
How T3 Gets Made
The thyroid takes iodine from the bloodstream and binds it to thyroglobulin. After several steps, T3 and T4 are produced.Only 20% of T3 is made directly in the thyroid. The liver (and kidneys to a lesser extent) produce the remaining 80% by converting T4 to T3. Liver function is critical here; poor liver health directly impairs T3 production.
Key nutrients for production and conversion: Iodine (production), selenium (T4-to-T3 conversion enzyme activity), iron. Most people are low in iodine and selenium. Use iodised salt (don't overconsume). Selenium is directly required by the deiodinase enzymes that convert T4 to T3.
TSH (Thyroid Stimulating Hormone)
The brain constantly monitors T3 and T4. When levels drop, the hypothalamus releases TRH → pituitary releases TSH → thyroid produces more T3 and T4.Low T3/T4 isn't always a thyroid problem. It can be low TSH or low TRH.
- Hypothyroid: Insufficient T3/T4. High TSH with low T3 and T4 indicates the problem is in the thyroid itself.
- Hyperthyroid: Excess T3/T4. Seen with low TSH and high T3/T4. Low TSH with good hormone levels is actually favourable. If T3 and T4 get too high, it may indicate tissues are rejecting these hormones, a sign of metabolic dysfunction.
T3 Symptom Checklist
- Healthy T3: Good cold tolerance, warm baseline temperature, stable mood, new mitochondria production, improved lipid profile, optimal GH/IGF-1, good bone remodelling, strong reproductive health, good muscle protein synthesis, fast digestion, fast thinking and reaction time, dense eyebrows, long eyelashes.
- Low T3: Cold hands and feet, low energy, dry skin, thin hair, thinning eyebrows, slow pulse, brain fog, muscle cramps, slow digestion, slow reaction time.
- High T3: Anxiety, racing heart, unexplained weight loss, mood swings, constant sweating, diarrhoea, insomnia.
At-Home T3 Assessment
- Pulse: Resting heart rate should be around 90 BPM when fasting, with a body temperature around 37°C (98.6°F).
- Hands and feet: Persistent coldness or poor cold tolerance suggests low T3.
- Eyebrows: Thinning outer eyebrows is a classic low-metabolism marker. Dense eyebrows indicate healthy T3.
- Achilles tendon reflex test:
- Sit in a chair so your feet hang freely.
- Tap the Achilles tendon and watch the rebound.
- Fast return to resting position: healthy metabolism.
- Slow, sluggish return: low T3 indicator.
Increasing T3
- To Raise: Iodine, selenium, iron, zinc, magnesium, vitamin D, vitamin A, vitamins B2/B6/B12, caloric surplus, high carb intake, resistance training, HIIT, losing excess fat, saturated fats, orange juice throughout the day, good sleep, healthy liver function, HCG (minor effect).
- Things That Lower T3: Glucocorticoids (cortisol), somatostatin, ghrelin, high estrogen, inflammation, ketogenic diet, low protein, overtraining, excessive dopamine, PUFAs, serotonin, prolactin, poor sleep, free fatty acids, tryptophan (balance with gelatin), cysteine (balance with gelatin), endotoxins, histamine, nitric oxide surges, fluoride, low calcium, high PTH, raw vegetables, low CO2, excess iodine, low salt intake, adrenaline dominance.
Dr. Ray Peat: For a deeper understanding of metabolism, energy flow, and thyroid function, start with Ray Peat. His life's work focused on exactly these topics. His articles are available at raypeat.com.
Aldosterone
To understand aldosterone, you need to understand the RAAS: the renin-angiotensin-aldosterone system.Angiotensin is converted into angiotensin I by renin, then into angiotensin II by ACE. Angiotensin II stimulates aldosterone production.
What the RAAS controls: Sodium reabsorption, water retention, potassium excretion, blood pressure regulation. This system matters for appearance, specifically water retention and bloat.
Angiotensin can also promote inflammation and osteoclast activity, contributing to bone degradation. The anti-diuretic hormone ADH rises alongside aldosterone.
A dysregulated RAAS drives: Heart fibrosis, vascular damage, myocardial remodelling, elevated blood pressure, inflammation, chronic stress.
- Natural approach: 1:2 or 1:3 sodium-to-potassium ratio (athletes use 1:2), adequate hydration, physical activity and sweating.
- On potassium loading for debloating: It doesn't work. When potassium rises, aldosterone increases to preserve sodium and prevent dehydration. Flooding your system with potassium triggers more sodium reabsorption and potassium excretion, the exact opposite of what you want. Bloat is driven by GH, estrogen, aldosterone, and fluid intake. No potassium supplement overrides those.
- Pharmaceutical options: Telmisartan (angiotensin II receptor blocker), Eplerenone (mineralocorticoid receptor antagonist, blocks aldosterone's effects directly).
Melatonin
Melatonin prepares the body for sleep. It doesn't create tiredness (adenosine does that), but it signals every organ that it's time to wind down. Without adequate melatonin, reaching deep sleep is difficult, which directly impacts GH, testosterone, and overall hormonal recovery.Other Effects:
- Potent antioxidant, protects mitochondria from oxidative stress, potential anti-ageing effects
- Decreases insulin sensitivity at night (pancreatic melatonin receptors)
- Lowers blood pressure at night
- Reduces fat production
- Raises GH secretion
- Increases bone density (bones have melatonin receptors)
- Modulates the immune system
How Melatonin Is Made
- Tryptophan
- 5-HTP
- Serotonin
- N-acetylserotonin
- Melatonin
- Other ways to raise melatonin: Blue light blocking glasses, dimmed evening lighting, morning sunlight exposure, lower cortisol, no caffeine 8-10 hours before bed, morning workouts, pistachios, tart cherry, low-dose melatonin supplementation.
On melatonin supplementation: It does not suppress natural production. Melatonin synthesis is primarily driven by the light-dark cycle. Exogenous melatonin has no lasting impact on endogenous output, and there are no withdrawal effects.
Oxytocin
Oxytocin is produced in the hypothalamus and acts as both a hormone and neuromodulator. It's most active during social interaction.Effects: Social awareness, empathy, emotional bonding, emotional regulation, trust, situational awareness, emotional intelligence, sexual function, pain reduction, heart protection, lower blood pressure, reduced inflammation in the gut, improved gut motility, reduced food intake, increased bone formation, increased DHT.
Note: That last point is worth emphasising. Social isolation literally lowers your androgen levels.
- Increasing Oxytocin:
- Lifestyle: Warm environments, exercise, martial arts training, slow breathing, meditation, singing, laughing, playing with a pet, adequate sleep, time in nature.
- Nutrition: Magnesium, vitamin C, taurine, tryptophan, probiotics, omega-3, vitamin D, zinc, dark chocolate.
- What Suppresses Oxytocin: Chronic stress, social isolation, trauma, sleep deprivation, high estrogen, inflammation, imbalanced gut microbiome, alcohol, opioids, SSRIs.
Cholecystokinin (CCK)
CCK illustrates how tightly the gut and brain are connected. It's secreted from cells in the small intestine when protein and fat are being digested. It also acts as a neuropeptide with significant effects on stress.CCK influences the testes, pituitary, thyroid, and adrenal glands.
- Effects: Increases satiety, increases prolactin, decreases GH (via somatostatin release), increases stress, improves nutrient absorption, supports proper digestion, supports reward signalling.
- What raises CCK: Protein, fat, bitter foods, coffee, tryptophan, phenylalanine, potatoes.
- What lowers CCK: Low protein diet, low fat diet, trypsin before meals, MCT oil (coconut oil), carrots.
Cortisol
Cortisol is released via: CRH (hypothalamus) → ACTH (pituitary) → Cortisol (adrenal glands)Cortisol in the Brain
At moderate concentrations, cortisol activates mineralocorticoid receptors (MR/NR3C2), which have high affinity. MR activation drives arousal and vigilance, important for waking up and cognitive function. The cortisol rise 30-45 minutes after waking is normal and useful.At higher levels, low-affinity glucocorticoid receptors (GR/NR3C1) activate. These trigger the full stress response: habitual threat vigilance, impaired self-control, and reactive thinking. This made sense evolutionarily; survival required fast, automatic responses.
- Glutamate and GABA: GR activation increases glutamate release, increases NMDA/AMPA receptor trafficking (more excitability), reduces GABA-A activity, chronically reduces BDNF in hippocampus and prefrontal cortex while strengthening amygdala output.
- Monoamines: Cortisol increases norepinephrine and dopamine synthesis, and upregulates β-adrenergic receptors in the amygdala, amplifying future stress responses.
Cortisol in the Body
- Muscle: Acutely, the cortisol spike from exercise is necessary and anabolic; it mobilises amino acids and glucose to support training. Do not work out late at night; cortisol spikes at the wrong time confuse the circadian rhythm and impair recovery and muscle gains.
- Chronically Elevated Cortisol: Blunts mTOR, increases proteolysis (muscle breakdown), suppresses satellite cells, decreases myogenesis, increases atrophy (particularly fast-twitch type 2 fibres; you lose strength, speed, and power before endurance).
- Bone: Reduces bone mineral density, blunts bone growth, reduces osteoblast survival and activity, increases RANKL and osteoclast-driven bone breakdown.
Lowering Cortisol
The primary mechanism is increasing GABAergic activity; GABA is the main inhibitory neurotransmitter.- GABA-supporting compounds: Magnesium, taurine, glycine, gelatin powder, valerian root, lemon balm, nettle tea, testosterone, L-glutamate, DHT.
- Lifestyle: Train in the morning, high-carb diet, eat carbs around training (counteracts mTOR suppression), recover properly (overtraining chronically elevates cortisol), optimise your circadian rhythm, no alcohol, no caffeine within 8-10 hours of bed, stay hydrated with adequate electrolytes and sodium.
- Supplements: Omega-3, creatine, magnesium bisglycinate, phosphatidylserine, collagen powder, electrolytes.
- Pharmaceuticals: Telmisartan, eplerenone.
Cortisol Timing
- Melatonin and Cortisol: Melatonin and cortisol are direct antagonists. When one rises, the other falls. Lowering evening cortisol improves sleep onset and sleep quality.
- Working Out at Night: Cortisol rises during training as part of the normal anabolic response. At night, cortisol's half-life extends slightly (approximately 15-30 minutes longer than earlier in the day), meaning it stays elevated when you need to wind down. Training at night also impairs insulin sensitivity and nutrient partitioning, both of which are naturally optimal in the earlier hours of the day.
Result: Food isn't properly digested, cortisol inhibits recovery, nutrients are partitioned toward fat storage rather than muscle. Train in the morning.
Parathyroid Hormone (PTH)
PTH regulates the calcium-to-phosphorus (CaP) ratio in the body. It rises when calcium is low or phosphorus is too high.When blood calcium drops - PTH rises - calcium gets pulled from bone.
This is why calcium intake matters. Phosphorus is high in meat and dairy, so prioritising high CaP ratio foods is important.
- High CaP ratio foods: Kale, dairy, kefir, yoghurt, cheese.
- Main PTH regulators: Calcium, phosphorus, vitamin D. (To raise vitamin D: fatty fish, sunlight, eggs, adequate magnesium).
Practical action: Blend an eggshell into powder and drink it with water. Boil or bake the shell first (10 minutes) to kill bacteria. One shell delivers roughly 1g of calcium.
Vitamin D also strongly regulates PTH. Even with good dietary calcium, low vitamin D will raise PTH.
Pulsatile vs. Chronic PTH
PTH pulses roughly 6 times per hour. Short pulses are beneficial for bone. Chronic elevation of PTH promotes bone breakdown: it stimulates osteoblasts and osteocytes to produce RANKL, which activates osteoclasts. Duration, not just level, determines whether PTH builds or breaks bone.Prolactin and PTH
The pituitary has PTH receptors. When PTH stays chronically elevated, it reaches the pituitary and stimulates prolactin secretion. Another reason adequate calcium intake matters beyond just bones.IGF-1
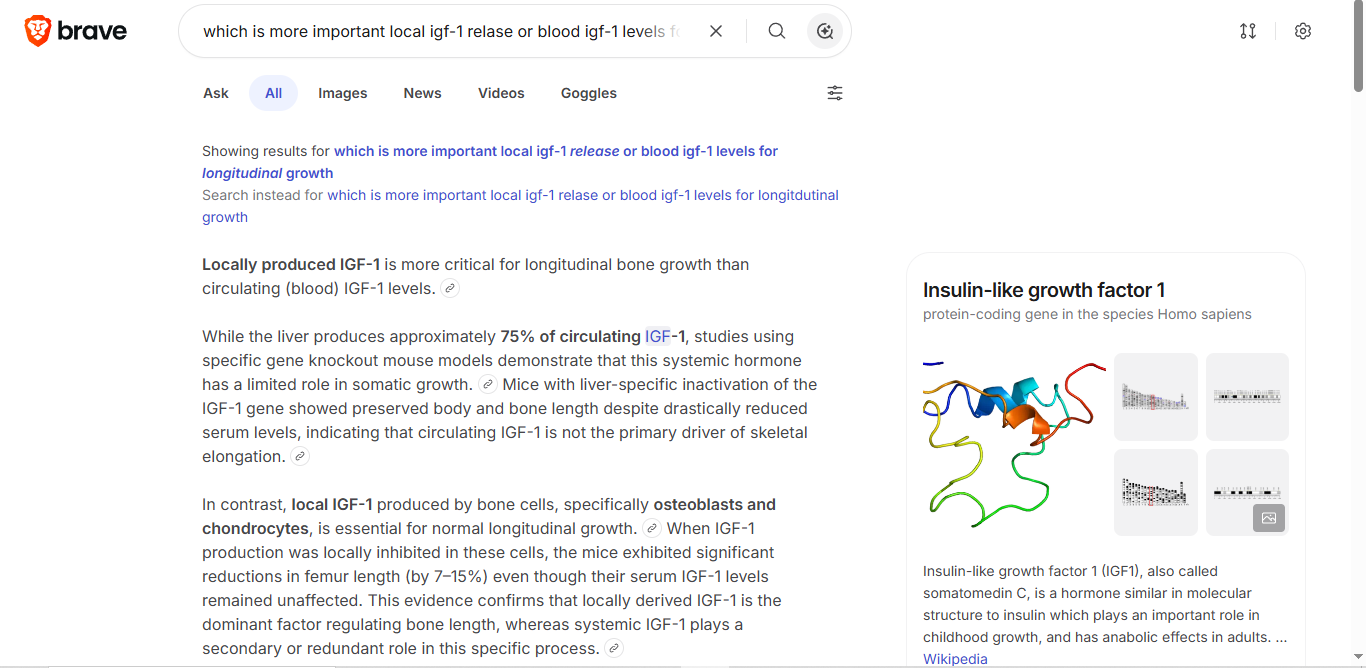
IGF-1 is responsible for the majority of GH's anabolic and growth-promoting effects. It's produced in the liver (via direct GH stimulation) and locally in tissues like the growth plates. To reach target tissues when not locally produced, IGF-1 is carried by IGFBP proteins, specifically IGFBP3 for the growth plates.Note: IGF-1-LR3 is immune to IGFBP binding, making it useless for height growth specifically.
What IGF-1 Does:
- Primary driver of height growth (stimulates chondrocyte proliferation and hypertrophy)
- Direct anabolic effects in muscle, bone, and other tissues
- Binds the insulin receptor at high concentrations and hybrid IR/IGF-1 receptor complexes
- Responsible for the pump from IGF-1-LR3 and similar compounds
- Negatively modulates GH secretion (high IGF-1 suppresses GH)
- Strongly correlated with IQ and brain development
- Directly neuroprotective and neurotrophic, supports synaptic plasticity, learning, and brain health
Increasing IGF-1
The most effective approach is optimising GH secretion and GH-to-IGF-1 conversion (see GH section).- Additional direct supports: Dairy, zinc, sleep quality, creatine, HIIT, colostrum, raw goat milk, caloric surplus, high protein diet, carbohydrates, testosterone, healthy thyroid.
- What decreases IGF-1: Caloric restriction, poor sleep, fasting, low protein diet, vegan diet, liver dysfunction, cortisol, prolactin, myostatin.
Nutrition Reference
Best dietary sources for every nutrient mentioned throughout the guide.| Nutrient | Best Sources |
| Apigenin | Onions, chamomile tea |
| Betaine | Quinoa, shrimp |
| Boron | Prunes, raisins |
| Choline | Eggs |
| Chrysin | Bee pollen, passionflower tea |
| Cholesterol | Butter, red meat, eggs |
| CoQ10 | Beef heart, royal jelly |
| Creatine | Red meat, herring, supplement |
| Cysteine | Eggs, beef, fish |
| EGCG | Green tea |
| Glycine | Gelatin powder, bone broth, collagenous meat |
| L-Lysine | Meat, fish, dairy |
| L-Phenylalanine | Eggs, fish, meat |
| L-Theanine | Green tea, black tea, supplement |
| L-Tyrosine | Red meat |
| Leucine | Protein powder, milk |
| Magnesium | Avocado |
| MCT | Coconut oil |
| Naringin | Oranges, kiwi, grapefruit |
| Omega-3 | Salmon, mackerel |
| Ornithine | Meat, fish, dairy |
| Phosphatidylserine | Liver, kidney, fatty fish |
| Polyphenols | Pomegranate juice, oranges, blueberries |
| Potassium | Pomegranate juice, bananas, avocado |
| Quercetin | Onions, apples |
| Resveratrol | Grapes, berries |
| Selenium | Shellfish, red meat |
| Taurine | Red meat |
| Thiamine (B1) | Orange juice, beef heart, salmon |
| Vitamin A | Liver, egg yolk, carrots, sweet potato |
| Vitamin B2 | Goat dairy, beef liver |
| Vitamin B3 | Chicken breast, tuna, coffee, royal jelly |
| Vitamin B5 | Avocado, shiitake mushrooms, eggs, bee pollen |
| Vitamin B6 / P5P | Liver, banana, royal jelly |
| Vitamin B9 | Avocado, liver, nattokinase |
| Vitamin B12 | Eggs, dairy, beef, lamb, clams, mussels |
| Vitamin C | Citrus fruits, berries |
| Vitamin D | Fatty fish, sunlight |
| Vitamin E | Olive oil, mango, tomatoes |
| Zinc | Mussels, oysters |
Last edited: